Chronic Illness and Disability: A Multisystemic Practice Model*
Abstract
Serious health conditions can severely strain family relationships. This article describes the Family Systems Illness (FSI) model to provide a guiding framework to help individuals, couples, and families navigate the changing landscape in the experience of illness and disability over time. This resilience-oriented practice approach distinguishes three dimensions of the illness experience and trajectory over time: (a) “psychosocial types” of health conditions, based on the pattern of onset, course, outcome, disability, and level of uncertainty; (b) major developmental phases in their evolution over time (initial crisis, chronic, terminal), facilitating longitudinal thinking about chronic conditions as an ongoing process with transitions and changing demands; (c) key family system variables, emphasizing: the interweaving of illness, individual, and family development; multigenerational themes and legacies related to illness and loss that influence coping and adaptation; family health belief systems (e.g., meaning-making, including influences of culture, ethnicity, spirituality, gender, and race), and the goodness of fit in the patient/family/health care provider relationship. The FSI model is intended for a broad spectrum of health conditions in children and adults, diverse health care professional disciplines, and clinical settings. Discussion includes timely, cost-effective applications in different clinical settings, including the use of prevention-oriented family consultations, psychosocial checkups, and brief and intensive interventions.
Introduction
Illness, disability, and death are universal family experiences. The questions are when in our lives they will occur, under what conditions, how serious they will be, and for how long. Perhaps most salient is how the experience will affect couple and family bonds and shared goals and dreams. With major advances in medical technology, individuals with adequate health care access are living much longer and better with conditions that historically have been fatal. Ever-growing numbers of families are living with chronic conditions over an increasingly long timespan and coping with multiple disorders, often simultaneously (Boersma et al., 2020). This article provides a family systems-based, normative, preventive model for psychoeducation, assessment, and intervention with families facing chronic and life-threatening conditions. The Family Systems Illness (FSI) model offers a systemic view of healthy family adaptation to serious illness as a developmental process over time in relation to the diversity and complexities of contemporary family life.
Over the past four decades, family-centered, collaborative, biopsychosocial-spiritual models of health care have grown and evolved (Knafl et al., 2021; McDaniel et al., 2013, 2014; Miller et al., 2006; Peek, 2015; Rolland, 1994a, 2018; Talen & Burke, 2013; Wood et al., 2021; Wright & Bell, 2009, 2021). There is substantial evidence for the mutual influence of family functioning, health, and physical illness (D’Onofrio & Lahey, 2010; Proulx & Snyder, 2009; Umberson & Thomeer, 2020; Weihs et al., 2002) and the usefulness of family-centered interventions with chronic health conditions (Berry et al., 2017; Campbell, 2003; Gilliss et al., 2019; Hartmann et al., 2010; Kazak, 2006; Lamson et al., 2022; Martire et al., 2010; Ruddy & McDaniel, 2024; Shields et al., 2012; Sousa et al., 2021). These systematic reviews summarize the increasing body of research regarding the impact of serious illness on families across the lifespan and the relationship of family processes to illness behavior, adherence, and course.
We need a comprehensive way to organize our thinking about the myriad complex interactions between biological diseases, patients, family members/caregivers, and involved health care providers. We need a model that can accommodate the changing landscape of interactions between these “parts of the system” over time.
Most families enter the world of illness and disability without a psychosocial map. Needed family system-oriented education and interventions, and national policies to support these families are often lacking. To create a normative context for their illness experience, families need the following foundation. First, families need to understand themselves as a systemic functional unit. Second, they need a systemic psychosocial understanding of the condition. This means learning the expected pattern of practical and affective demands of a disorder over its course. This includes a timeframe for disease-related developmental tasks associated with different phases of the unfolding disorder. Third, they need an appreciation of individual and family life course patterns and transitions to facilitate their incorporation of changing developmental priorities for the family unit and individual members in relation to evolving challenges of a chronic disorder. Finally, families need to understand the cultural, ethnic, spiritual, and gender-based beliefs that guide the type of caregiving system and meanings they create.
Overview of FSI Model
How can we bring together this large and complex landscape in a manner useful to affected families and clinical practice? The FSI model (Rolland, 1987, 1990, 1994a, 1994b, 2016, 2018) offers a beneficial framework for assessment and intervention with families facing chronic illness and disability. The FSI Model can be applied to a full range of adult and childhood-onset illnesses and disabilities, including neurocognitive and genomic conditions (Rolland, 2017; Rolland & Williams, 2005).
The FSI model is grounded in a resilience orientation, viewing family relationships as a potential resource and emphasizing possibilities for growth, not just their liabilities and risks (Walsh, 2016). A broad range of family forms and processes are considered normative. Taking the family as the interactive hub, the FSI model conceptualizes a systemic interaction between an illness and family that evolves over time. The goodness of “fit” between the psychosocial demands of the condition over time and the family style of functioning and resources is a key determinant of effective versus dysfunctional coping and adaptation.
The FSI model has three dimensions: (a) a psychosocial typology of chronic conditions; (b) major time phases in their evolution; and (c) key family system components (Figure 1). In addition to communication processes and organizational/structural patterns, family components given particular emphasis include family and individual life course development, particularly in relation to the time phases of a disorder; multigenerational legacies related to illness and loss; and belief systems (including influences of culture, ethnicity, spirituality, and gender).
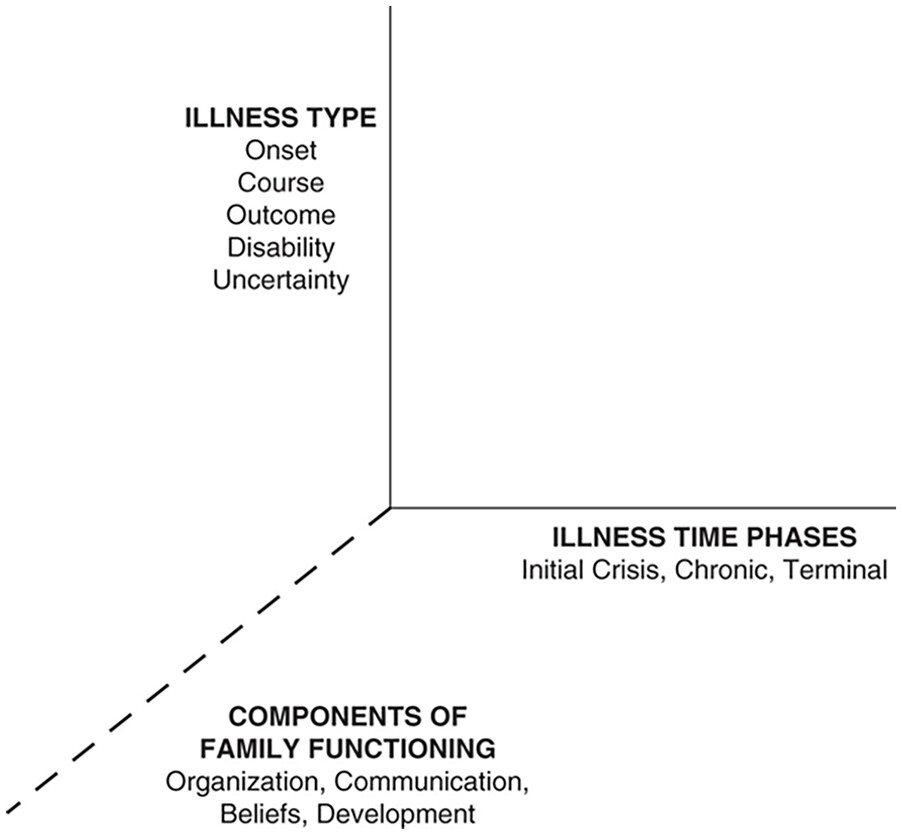
Figure 1. Family Systems Illness Model: Three Dimensions.
From Rolland (2018). Reprinted by permission of Guilford Press.
Psychosocial Types of Illness
The standard disease classification is based on purely biological criteria clustered to establish a medical diagnosis and treatment plan, rather than the psychosocial demands on patients and their families. This article provides a different classification scheme that offers a better bridge between the biological and psychosocial worlds, and thereby clarifies the relationship between chronic conditions and families (Rolland, 2018). The goal of this typology is to provide meaningful and useful categories with similar psychosocial demands for a broad range of chronic conditions across the lifespan. Illness patterning can vary in terms of: (a) onset, (b) course, (c) outcome, (d) type and degree of disability, and the (e) level of uncertainty about its trajectory.
Onset
Illnesses can have either a more acute clinical onset, such as a heart attack, or a more gradual onset, such as Parkinson’s disease. For acute onset conditions, emotional and practical changes are compressed into a short time, requiring more rapid family mobilization and crisis management skills. In such situations, families need to be helped to tolerate highly charged emotional situations, exchange roles flexibly, problem-solve efficiently, and utilize outside resources.
Course
The course of chronic diseases can take three general forms: progressive, constant, or relapsing/episodic. With a progressive disease, such as metastatic cancer, disability worsens in a stepwise or gradual way. The family typically lives with perpetual symptoms and the prospect of continual relationship and role changes as the disease progresses. Increasing strain on family caregiving is caused by exhaustion with few periods of relief from illness demands and by new caretaking and financial challenges over time.
With a constant-course illness, the occurrence of an initial event, such as a single heart attack or spinal cord injury, is followed by a stable biological course. Typically, after an initial period of recovery, the illness is characterized by some clear-cut deficit or limitation. The family is faced with a semi-permanent change that is stable and predictable over a considerable time span. The potential for family exhaustion exists without the strain of new role demands over time. For example, a man with a spinal cord injury paralyzing him from the waist down was able to devise a slow, methodical plan to return to work within 2 years. This plan, which depended largely on a predictable illness trajectory, required the family to establish and follow a realistic program.
A relapsing or episodic course illness, such as back problems or asthma, is distinguished by the alternation of stable low symptom periods with periods of flare-up or exacerbation. Families are strained by both the frequency of transitions between crisis and noncrisis, and the ongoing uncertainty of when a recurrence will occur. This requires family flexibility to alternate between two patterns of family organization. The wide psychological discrepancy between low symptom periods versus flare-up is particularly taxing.
Outcome
The extent to which a chronic illness leads to death or shortens one’s life span has profound psychosocial impact. The continuum ranges from illnesses that do not typically affect the life span to those that are progressive and usually fatal, such as metastatic cancer. An intermediate, more unpredictable category includes both illnesses that can shorten the life span such as heart disease, and those with the possibility of sudden death such as hemophilia. A major difference between these kinds of outcome is the degree to which the family experiences anticipatory loss and its pervasive effects on family life (Rolland, 1990, 2018).
Disability
Disability can involve cognitive impairment (e.g., acquired brain injury), sensation (e.g., deafness), movement (e.g., multiple sclerosis), stamina (e.g., heart disease), disfigurement (e.g., mastectomy), and those associated with social stigma (e.g., HIV). The degree, kind, and timing of disability typically affect the level of family stress. For instance, combined cognitive and motor deficits caused by a major stroke generally necessitate greater family reorganization than a condition without cognitive impairment. For progressive diseases, like Alzheimer’s disease, cognitive disability looms as an increasing problem in later phases of the illness, allowing a family more time to prepare for anticipated changes and an opportunity for the ill member to participate in disease-related family planning while still cognitively able (Boss, 2011).
Uncertainty
The predictability and degree of uncertainty about the specific way or rate at which a disease unfolds overlays all other variables. For illnesses with highly unpredictable courses, such as multiple sclerosis, family coping and future planning can be hindered by anticipatory anxiety and ambiguity about what family members will actually encounter. Families able to put long-term uncertainty into perspective are best prepared to avoid the risks of exhaustion and dysfunction. For conditions with long-range risks, including genomic disorders, families can maintain mastery in the face of uncertainty by enhancing the capacity to acknowledge the possibility of loss, sustain hope, and build flexibility into both the family’s and each member’s life course planning that conserves and adjusts major goals and helps circumvent the forces of uncertainty (Rolland, 1990, 2006b).
By combining the kinds of onset, course, outcome and disability, and predictability into a grid, we generate a typology that clusters illnesses according to similarities and differences in patterns that pose differing psychosocial demands.
Time Phases of Illness
Frequently, conversations about “coping with cancer” or “managing disability” approach illness and disability as a static state and fail to appreciate the evolution of illness processes over time. The concept of time phase provides a way for clinicians and families to think longitudinally and to understand chronic illness as an ongoing process with normative landmarks, transitions, and changing demands. Each phase poses psychosocial challenges and developmental tasks that may require different strengths, attitudes, or changes for family adaptation. Core psychosocial themes in the natural history of chronic disease can be organized into three major phases: initial crisis, chronic, and terminal (Figure 2).
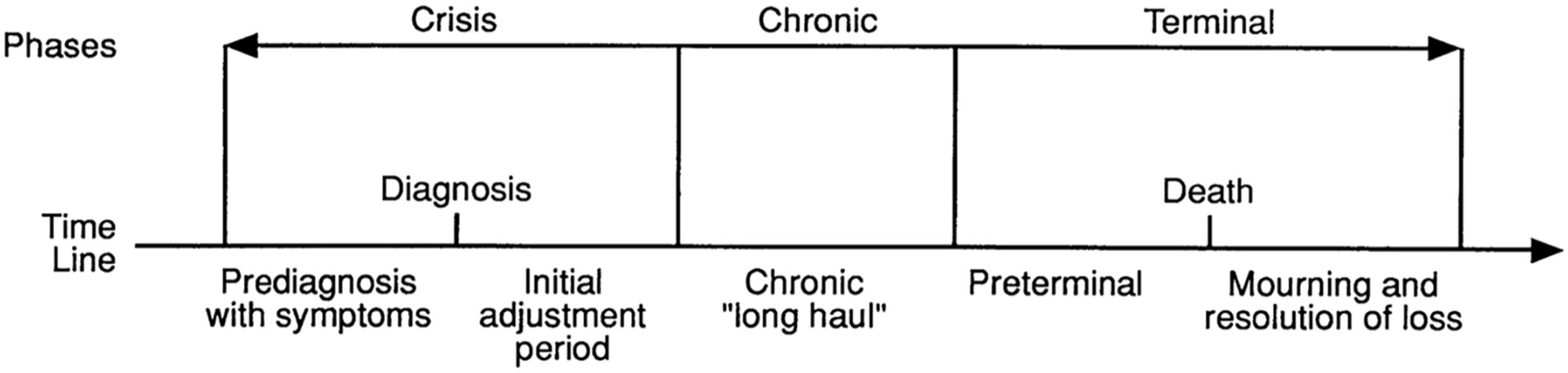
Figure 2. Timeline and Phases of Illness.
From Rolland (2018). Reprinted by permission of Guilford Press.
Initial Crisis Phase
The crisis phase includes any symptomatic period before diagnosis through the initial readjustment period after a diagnosis and initial treatment planning. This phase presents a number of key tasks for the ill member and family. These include (a) learning to cope with any symptoms or disability, (b) adapting to health care settings and treatment procedures, and (c) establishing and maintaining workable relationships with the health care team. Also, there are critical tasks of a more general, existential nature. Families optimize wellbeing when they can: (a) view the challenge of illness as a shared challenge in “WE” terms, (b) pull together to cope with the immediate crisis, (c) create illness meanings that promote family mastery and competence, (d) grieve for the loss of health, (e) gradually accept the illness as long-term while maintaining a sense of continuity between their past and future, and (f) in the face of uncertainty, develop flexibility toward future goals.
During this initial adjustment period, health care professionals have enormous influence over a family’s approach to and sense of competence and their strategies to accomplish these developmental tasks. Initial meetings and advice given at the time of diagnosis can be thought of as a “framing event.” Since families are so vulnerable at this point, clinicians need to be extremely sensitive in their interactions with family members. Families can interpret decisions about who is included or excluded (e.g., patient) from initial discussions as a message of how they should plan their illness-related communication going forward. For instance, if a clinician meets with parents separately from an adolescent to give them information about a cancer diagnosis and prognosis, they may assume they are being instructed implicitly to protect their adolescent from any discussion of the illness. Clinicians can ask patients about preferences and cultural norms related to who they would like to include in important discussions and about receiving information from providers.
With life-threatening conditions that can cause sudden death (e.g., heart attack), there is a higher premium on early frank conversation. Knowing an ill member’s wishes concerning heroic medical efforts and life support can benefit everyone. For example, in one family, the father had serious heart disease. Everyone, including the father, became emotionally paralyzed by fear because end-of-life decision-making had been avoided. Family consultations facilitated the father making his wishes known regarding the limits on life-saving efforts. This relieved his family members because they knew his feelings if they had to make life and death decisions. For the father, making his wishes known not only gave him a sense of personal control over the end of his life, but also freed his energy to focus on living well and maximizing his physical wellbeing. Despite the short-run challenge of having end-of-life discussions, it is important to keep in mind that many of the most wrenching end-of-life experiences for families occur when the wishes of a dying member are unknown or have been disregarded (Rolland et al., 2017). With conditions involving progressive dementia, such as Alzheimer’s disease, there is added incentive for conversations before the affected person’s cognitive impairment makes meaningful discussion impossible (Boss, 2011; Rolland, 2017).
Chronic Phase
The chronic phase can be marked by constancy, progression, or episodic change. It is “the long haul” or “day-to-day living with chronic illness” phase. Salient issues include (a) pacing and avoiding burnout; (b) minimizing relationship imbalances between the patient and other family members; (c) maximizing autonomy and preserving or redefining individual and family developmental goals within the constraints of the illness; and (d) sustaining relational connectedness in the face of threatened loss. The ability of the family to maintain the semblance of a normal life is a key task of this period. If the illness is potentially fatal, this is a time of “living in limbo.” For certain highly debilitating but not clearly fatal illnesses, such as a massive stroke or dementia, the family can feel saddled with an exhausting problem “without end.” Encouraging maximal autonomy for all family members in the face of prolonged adversity helps to offset trapped, helpless feelings.
For long-term disorders, customary patterns of intimacy for couples become skewed by discrepancies between the ill and the well spouse/caregiver (Rolland, 1994b, 2018). Ambivalent emotions often remain private and can contribute later to “survivor guilt.” As one young husband lamented about his wife’s cancer:
It was hard enough two years ago to absorb that, even if Sally was cured, her radiation treatment would make pregnancy impossible. Now I find it unbearable that her continued uncertain battle with cancer makes it impossible to go for our dreams like other couples our age.
Normative ambivalence and escape fantasies often remain underground and contribute to survivor guilt and prolonged grief. Psychoeducational couple interventions that normalize such emotions related to threatened loss can help prevent destructive cycles of blame, shame, and guilt.
When clinicians inquire about and validate the psychosocial burden of caregivers, especially well spouses, they help prevent the physical burden of the patient from becoming the only currency in family relationships. This approach facilitates families seeing a life-threatening illness as a shared challenge rather than solely the domain of the patient, a major contributor to dysfunctional family processes when living with a serious illness.
Terminal Phase
In the terminal phase, the inevitability of death becomes apparent and dominates family life. The family must cope with issues of separation, death, mourning, and beginning the reorganization process needed for resumption of family life beyond the loss (Walsh, 2023; Walsh & McGoldrick, 2013). Families adapt best to this phase when they can shift their view of hope and mastery from controlling the illness to a successful process of “letting go.” Optimal coping involves emotional openness as well as dealing with the myriad of practical tasks. This includes seeing this phase as an opportunity to share precious time together, to acknowledge the impending loss, to deal with unfinished business, to say goodbyes, and to begin the family reorganization process. If they have not determined beforehand, the patient and key family members need to decide about such things as a living will, the extent of medical heroics desired, who will serve as a legal proxy if the patient’s competency to make sound decisions is compromised (Rolland et al., 2017), preferences about dying at home, in the hospital, or an extended care facility, and wishes about a funeral or memorial service and burial or cremation.
Transitions Between Phases
Critical transition periods link the three time phases. These are times when families re-evaluate the appropriateness of their previous coping and adaptation in the face of new illness and disability-related challenges. Helping families address unfinished business from the previous phase can facilitate movement through the transitions. Families can become permanently frozen in an adaptive structure that has outlived its utility. For example, the usefulness of pulling together while deferring other life plans in the crisis phase can become maladaptive and stifling for all family members through the chronic phase.
Clinical Applications
The FSI model provides a framework for clinical practice by facilitating an understanding of chronic illness and disability in psychosocial terms. Attention to features of onset, course, outcome, and disability provides markers that focus clinical assessment and intervention with a family. An illness timeline delineates psychosocial developmental phases of an illness, each phase with its own salient developmental challenges. In particular, mastering initial crisis phase-related challenges provides a foundation for successful adaptation over the long haul. Attention to time allows the clinician to assess family strengths and vulnerabilities in relation to the present and future phases of the illness. The psychosocial demands of any condition can be thought about in relation to each illness phase and to different components of family functioning (e.g., communication, problem-solving, role flexibility).
The model clarifies treatment planning. Goal setting is guided by awareness of the aspects of family functioning most relevant to the particular type or phase of an illness. Sharing this information with the family and deciding on specific goals offers a sense of control and realistic hope. This process empowers families in their journey of living with a chronic disorder. Also, it educates family members about warning signs to alert them to seek help at appropriate times for consultation or brief, goal-oriented treatment. This framework is useful for timing family consultations or “psychosocial checkups” to coincide with key illness transition points.
The FSI model can be applied across disciplines by both health and mental health care providers, appreciating varied clinical settings and time constraints. Providers who function under enormous time pressures and have limited opportunities with families can adapt this approach to make the best use of their time. Asking a few well-chosen questions can serve as a “screening scan.” If a critical issue is identified, clinicians can decide whether to pursue it further or refer to an appropriate behavioral health colleague for more in-depth evaluation and intervention.
Assessment Components of Family Functioning
As chronic conditions become incorporated into the family system, illness-oriented family processes that concern the dimension of time and belief systems influence coping.
Multigenerational Legacies of Illness, Loss, and Crisis
A family’s current behavior, and therefore its response to illness, cannot be adequately understood apart from its history (Bowen, 2004; McGoldrick et al., 2016). A multigenerational inquiry helps to clarify areas of strength and vulnerability. It also identifies high-risk families, burdened by past, unresolved issues and dysfunctional patterns, that will need mental health care to absorb the challenges of a serious condition. Such inquiry helps explain the family’s current style of coping, adaptation, and meaning-making.
A chronic illness-oriented genogram (McGoldrick et al., 2020) focuses on how the current and previous generations organized and adapted over time to illnesses and unexpected crises. A central goal is to bring to light areas of consensus and “learned differences” that are sources of cohesion, resilience, and potential conflict. Patterns of coping, shifts in relationships (e.g., alliances, triangles, cutoff), and sense of competence are noted. These patterns can be transmitted across generations as family pride, myths, catastrophic expectations, and belief systems. In one case involving a couple in which the husband was diagnosed with basal cell carcinoma, the oncologist discussed a favorable prognosis. Despite this reassurance, the wife believed her husband would die from this skin cancer. This resulted in increased marital discord and ultimately the couple’s consultation with a behavioral health provider. In the consultation interview, when asked about prior experiences with illness and loss, the wife revealed that her own father had died tragically of a misdiagnosed malignant melanoma. This woman had a catastrophic fear based on both sensitization to cancer (particularly any related to the skin) and the possibility of human error by health professionals. Had the oncology team inquired about prior experiences at the time of diagnosis, earlier intervention would have been facilitated. Alternatively, positive family-of-origin experiences with illness, loss, and adversity can provide transferable sources of resilience and effective coping skills to adapt to the current situation (Walsh, 2016).
Interweaving of Individual, Family, and Illness Development
A developmental lens provides a powerful way to construct a normative framework for serious illness. To place the unfolding of chronic disease into a developmental context, it is vital to understand the intertwining of three evolutionary threads: illness, individual, and family development.
Concepts of human and family development have evolved from models that centered on a basic, somewhat invariant, sequence and unfolding of phases to ones that are more varied, fluid, and multidimensional, consistent with contemporary individual and family life course trajectories (Lerner, 2018; McGoldrick et al., 2016; Walsh, 2012). Serious health conditions are one example of major, often unexpected, life challenges that can significantly alter the sequence and character of a family’s and its members’ life course. Life structure, referring to the core elements in one’s life (e.g., work, childrearing, caregiving), is a useful central concept for both family and individual development. Illness, individual, and family development have in common the notion of phases, each with its own priorities and marked by the alternation of life structure stable and transitional phases (Levinson, 1986). In a transition phase, one weighs different possibilities for personal and family life, eventually drawing up blueprints for the next phase, and then living them out. The actual possibilities may be affected by assets or barriers related to culture, race, class, gender, and sexual orientation. Transition phases can be quite fluid. Previous individual, family, and illness life structures are reappraised in the light of new developmental challenges. Furthermore, typical family development moves between phases that require intense bonding and an inside-the-family focus, as in early childrearing, and phases during which the external family boundary is loosened, such as with emerging young adults, often emphasizing increased personal identity and autonomy.
These unifying concepts provide a foundation for understanding the experience of chronic disorders. Life course development alternates between transition and life structure stable phases. And particular phases require relatively greater or lesser degrees of family cohesion. Illness, individual, and family development each pose priorities and challenges that move through phases of being more or less in sync with each other.
Serious health conditions tend to push developmental processes toward transition and increased need for cohesion and teamwork. Analogous to the addition of a new family member, illness onset sets in motion an inside-the-family-focused process of socialization to illness. Symptoms, loss of function, the demands of shifting or acquiring new illness-related roles, and the fears of further disability and/or death all push a family to pull together.
The need for family cohesion varies enormously with different illness types and phases. The tendency for a disease to pull a family inward increases with the level of disability or risk of progression and death. Progressive diseases over time inherently require greater cohesion than, for instance, constant-course illnesses. The ongoing addition of new demands with illness progression keeps a family’s energy focused inward, often impeding members’ development.
In clinical assessment, a basic question is: What is the fit between the psychosocial demands of a condition and family and individual life structures and developmental tasks at a particular point in the life course? Also, how will this fit change as the course of the illness unfolds in relation to the family’s and each member’s development?
Any transition in individual or family life course development will tend to magnify issues related to existing and anticipated loss. Transition periods are often characterized by upheaval, rethinking of prior commitments, and openness to change. Such times often hold a greater risk for the illness to become either embedded or ignored in planning for the next life phase. During a transition period, the process of thinking through future commitments can bring to the forefront family norms regarding loyalty through sacrifice and caregiving. The following example highlights this point.
In one second-generation Latino family, the father, a factory worker and primary financial provider, had a heart attack. His rehabilitation was uneventful, included appropriate lifestyle modifications, and a return to work. The family, including the oldest son, age 15 years, seemed relatively unaffected. Two years later, his father experienced a second more life-threatening heart attack and became totally disabled. His son, now 17 years old, had dreams of going away to college. The specter of financial hardship and the perceived need for a “man in the family” created a serious dilemma for the son and the family, which surfaced with precipitously declining academic performance and alcohol abuse. There was a fundamental clash between the developmental issues of launching a child and the ongoing demands of a progressive, life-threatening type of heart disease on the family. Furthermore, there is a resurgence of fears of loss fueled not only by the recurrence but also its timing with a major developmental transition for the oldest son. The son may fear that if he were to move away, he might never see his father alive again. There was a clash between simultaneous transition periods: (a) the illness transition to a more disabling, progressive, and life-threatening course; (b) the adolescent son’s transition to emerging adulthood with individuation, leaving home, and educational pursuits; and (c) the family developmental transition from the “living with teenagers” to a “launching young adults” phase. It also illustrates the significance of the type of illness: one that was less incapacitating and life-threatening might have interfered less with individual and family developmental priorities. At the time of initial diagnosis, inquiry about anticipated major transitions over the next 3 to 5 years and discussing them in relation to the specific kind of heart disease and its related uncertainties would help avert a future crisis.
It is essential to situate these developmental issues in the context of cultural values, socioeconomic considerations, availability of family or community resources, and access to health care. In many cultures, as in this Latino family, a strong emphasis on loyalty to family needs would normatively take priority over individual goals, especially with a major illness or disability.
If the particular illness is progressive, relapsing, increasingly incapacitating, and/or life-threatening, then the unfolding phases of the disease will be punctuated by numerous transitions. In these situations, a family will need to alter its life structure more frequently to accommodate shifting and increasing demands of the disease. This level of demand and uncertainty keeps the illness in the forefront of a family’s consciousness, constantly impinging on its attempts to get back “in phase” developmentally.
The transition from the crisis to the chronic phase is the key juncture at which the intensity of families’ socialization to living with chronic conditions is often lessened. In this sense, it offers a window of opportunity for the family to reestablish or sometimes chart a “new normal” developmental course.
An overarching goal is to deal with the developmental demands of the illness while preserving family members’ own and the family’s development as a system over time. It is important to consider whose life plans were or might be canceled, postponed, or altered, and when plans put on hold and future developmental issues will be addressed. Using this framework, clinicians can anticipate developmental nodal points and offer prevention-oriented consultations. Family members can be helped to strike a healthier balance, with life plans that minimize feelings of guilt, over-responsibility, and hopelessness, and find family and external resources to enhance freedom both to pursue personal goals and to provide needed care for the ill member.
Health Beliefs
When illness strikes, families strive to create meaning for the illness experience that promotes competency and mastery (Kleinman, 2020; Rolland, 2018; Wright & Bell, 2009, 2021). Since serious illness is often experienced as a betrayal of our fundamental trust in our bodies and belief in our invulnerability, it can be a formidable challenge to make meaning with an empowering narrative. Health beliefs can help us grapple with the existential dilemmas of our fear of death and tendency to deny our own mortality. They offer an approach to new and ambiguous situations, such as serious illness, and serve as cognitive maps guiding decisions and actions (Hansson & Cederblad, 2004). Our appreciative inquiry into beliefs is a powerful foundation for collaboration with patients and families (Rolland, 1997; Wright & Bell, 2009, 2021). Growing research evidence shows that family members’ distress about illness and genetic risk is more closely associated with perceived risk or appraisals of seriousness than objective characteristics of the disease (Franks & Roesch, 2006).
As part of early consultation(s), particularly in the initial crisis phase, it is useful to inquire about key family beliefs that shape families’ meaning-making, purpose, and coping strategies. This includes family health beliefs about: (a) normative illness experience; (b) meanings attached to symptoms by a family, ethnic group, religion, or the wider culture (e.g., chronic pain) or specific diseases (e.g., HIV/AIDS); (c) mind–body relationship, mastery, control, and acceptance; (d) assumptions about what caused an illness and what can influence it’s course and outcome; (e) multigenerational factors that have shaped a family’s health beliefs and response to illness; (f) gender-related beliefs about expected roles and behavior; and (g) anticipated nodal points in illness, individual, and family development when health beliefs will likely be strained or may need to shift. Clinicians should also consider the fit of health beliefs among family members as well as between the family and health care provider system and wider culture (Kirmayer et al., 2015).
Normative Illness Experience
Illness beliefs about what is normative or dysfunctional can powerfully influence family adaptation. Family values that normalize psychosocial illness challenges without stigma facilitate their use of outside resources and maintain a positive identity. Help-seeking viewed as weak and shameful undercuts resilience and fosters suffering. Basically, with chronic conditions, difficulties are to be expected; mental health care and outside resources are often needed.
Two beneficial questions to elicit these beliefs are: (a) “How do you think other families would typically deal with a similar situation to yours?” and (b) “How do you think families ideally cope with your situation?” Families with strong beliefs in high achievement and perfectionism are prone to applying norms that are incredibly difficult to achieve with chronic conditions. Especially with untimely conditions that occur in childhood through early adulthood, there are additional pressures to keep up with socially expectable developmental milestones of age peers. The fact that developmental goals may take longer or need revision requires a flexible belief about what is normal and healthy. This kind of flexibility helps sustain hope.
Ethno-Cultural and Spiritual Beliefs
Ethno-cultural, racial, and spiritual beliefs and dominant societal norms can strongly influence family values, concerns about health and illness, and their pathways in healing (Falicov, 2015; Kirmayer et al., 2015; Koenig, 2012; Rolland, 2006a; Walsh, 2010; Wright, 2017). Significant ethno-cultural differences regarding health beliefs often emerge during a major health crisis. Since American families frequently represent a blend of different ethnic, racial, and spiritual beliefs, health care providers need to be mindful of the diverse belief systems of various subpopulations in their communities, particularly as they are often expressed in different behavioral patterns. For instance, cultural and religious values and expectations can vary as to: (a) the appropriate “sick role” for the patient; (b) the kind and degree of open communication about the condition and prognosis; (c) who should be included in the illness caregiving system (e.g., extended family, friends, professionals); (d) gender-based expectations for caregiving and the primary caregiver (most often wife /mother/daughter/daughter-in-law); (e) which treatment or healing approaches can be helpful [e.g., Western medical experts, faith healing practitioners, mindfulness meditation (Kabat-Zinn, 2023), Eastern or indigenous traditional beliefs about illness etiology and curative practices]; (f) proper rituals at different illness phases (e.g., hospital bedside vigils, healing, and funeral rituals); and (g) within-family diversity (e.g., parents’ Spanish and Mexican cultural differences in handling a son’s diabetes). It is especially important to be mindful of beliefs with racial minority groups (e.g., African American, Asian, Hispanic) that experience discrimination or marginalization from prevailing Euro-American culture.
Clinicians need to be mindful of cultural and religious differences between themselves, the patient, and the family to forge a workable alliance through a long-term condition. Effective collaboration occurs when providers inquire into families’ cultural and spiritual beliefs about illness and healing. Disregarding these issues can lead families to distance themselves from health care providers and available community resources—a major source of adherence issues and treatment failure. Sometimes, providers need to flexibly modify their professional ethos to be “in charge.” This entails tolerance that patients, not health care providers, retain final decision-making about their bodies.
Beliefs About Mastery and Control Facing Illness
It is beneficial to inquire how a family defines mastery or control in general and particularly with illness. A family may hold different beliefs about control when dealing with some diseases in contrast to other life challenges. By example, regardless of the actual severity or prognosis in a particular case, cancer may be equated with “death” or “no control” because of medical statistics, cultural myth, or family history. In contrast, families may have enabling stories about a relative or friend, who despite cancer and a shortened lifespan, lived a “full” life centered on effectively prioritizing the quality of relationships and goals. Clinicians can highlight such positive narratives to help counteract cultural beliefs that may equate success with control over a disease.
A family’s beliefs about control can affect treatment adherence and the family’s participation in a member’s treatment and healing process. When patients view disease course or outcome as a matter of chance or beyond their control, they tend to establish marginal collaboration with health care providers and may not adhere to treatment recommendations. When poor minority families receive inadequate or lack access to care, it often fosters a fatalistic attitude and minimal engagement with providers, who may not be trusted. Because any therapeutic relationship depends on shared beliefs about what is therapeutic, it is essential to establish a workable accommodation of core beliefs among the patient, family, and health care team. Families that feel misunderstood by health care providers are often reacting to a lack of collaboration at this basic value level.
The quality of fit between family beliefs about mastery and the relative need for provider and technological care can vary with the illness phase. For some conditions, the crisis phase involves protracted care outside the family’s direct control. This may be stressful for a family that prefers to tackle its own problems without outside involvement and control. The patient’s return home, often part of the transition to the chronic phase, allows members to reassert their competence and leadership more fully. By contrast, a family that is more comfortable with intense involvement by health care providers might experience more difficulty when their ill member returns home from a rehabilitation facility, losing their locus of competency, the professional caregiving system. Appreciation of such normative differences in beliefs about control helps guide an effective psychosocial treatment plan tailored to family preferences.
Family Beliefs About Illness and Disability Etiology
When a major health issue arises, most of us question, “Why me (or us)?” and “Why now?” (Roesch & Weiner, 2001). We try to develop an explanation or story that helps organize our experience. With the limits of current medical knowledge and immense uncertainties about the relative importance of myriad factors, individual members and families construct diverse causal attributions about a condition. Beliefs about etiology need consideration separately from beliefs about what can affect the outcome. It is vital to inquire about each family member’s perspective. Various explanations may include the biological (e.g., virus), religious, societal (e.g., poverty or pollution), or individual or family dysfunction. Beliefs about etiology can include punishment for earlier misdeeds (e.g., an affair, an ancestor’s transgressions), blame of a particular family member (“Your nagging gave me a heart attack!”), a sense of injustice (“Why am I being punished”), genetics (e.g., heart disease runs on one side of the family), negligence by the patient (e.g., smoking) or by parents (e.g., sudden infant death syndrome), religious beliefs (God’s punishment for sinful living), or simply bad luck. Inquiry about culturally based beliefs or syndromes is valuable. For instance, Latino families may believe that nervios, an increased susceptibility to stress and symptoms of nervousness, has caused a cancer.
Optimally, family narratives respect the limits of scientific knowledge, affirm basic competency, and promote the flexible use of multiple biological, psychosocial-spiritual healing strategies. In contrast, causal attributions that invoke blame, shame, or guilt are particularly important to uncover, as they can derail family coping and adaptation. With a life-threatening illness, a blamed family member may be held accountable if the patient dies (e.g., “You neglected his care!”). Decisions about treatment can become confounded and filled with tension. The following case vignette illustrates how self-blame may remain hidden and the importance of early inquiry by health care providers:
Anne and Jack, a young couple, have one child Ellen, aged 5, who is terminally ill with leukemia. The pediatric oncologist has offered the parents the choice between an experimental treatment with a low probability of success, or halting treatment. Jack’s position is “Let’s stop; enough is enough.” Anne, on the other hand, felt, “We must continue; we can’t let her die.” The couple cannot reach an agreement, and the physician is immobilized. She requests a consultation for the couple.When asked, “How do you each try to explain or make sense of how your daughter got leukemia?” critical stories emerge. Jack basically sees it as bad luck. Anne, however, has a very different belief. During her pregnancy with Ellen, Anne’s father had a heart attack and died several months later from a second episode. Anne experienced this as a time of great stress and grief, which she felt adversely affected Ellen’s intrauterine life. After Ellen’s birth, by normal delivery, Anne was still mourning the loss of her father and feels that this negatively affected the quality of her bonding with Ellen and led to a hidden depression in her infant. Further, Anne had read research linking depression with decreased immune system effectiveness, which could then decrease normal surveillance and clearing of cancer cells from the body. She believes this combination of factors caused her child’s cancer and that if she had been a more competent mother, this never would have happened. Anne said she had never told this story to anyone, including her husband, because no one had ever asked, and she was very ashamed. She had hoped for a cure, so that the whole issue could be resolved. She could not accept stopping treatment because, to her, it meant that Ellen’s death would then be her fault. This wrenching situation could have been averted had someone on the healthcare team inquired early on regarding any beliefs about the etiology of Ellen’s cancer. Early timely referral to a family therapist would have been optimal.
Belief System Flexibility
Because illnesses vary enormously in their physiological responsiveness to psychosocial factors, both families and providers need to distinguish beliefs about (a) overall participation (or active agency) in a long-term disease process and (b) ability to control the biological progression and outcome. Families’ experience of competence often depends on their grasp of these distinctions. Mindful of advances in positive psychology (Carr et al., 2024), optimal family, and provider narratives respect the limits of scientific knowledge, affirm basic competency, and promote the flexible use of multiple biological and psychosocial healing strategies.
Clinicians can encourage a family’s flexible involvement in the overall illness and treatment process independent of whether a disease is stable, improving, or in a terminal phase. Proactive efforts to influence the course can make a difference, such as when parents stop serving sweet desserts, so as not to tempt an adolescent with diabetes. If an ill member gets a cancer recurrence and enters a terminal phase, involvement as an expression of mastery transitions from influencing the outcome to easing suffering and supporting palliative care.
Flexibility within the family and the health care team is a key variable in optimal functioning. Rather than linking mastery in a rigid way with biological outcome (survival or recovery), families can define mastery in a more “holistic” sense. Involvement in the overall process can be the main criteria of success. Psychosocial-spiritual healing may influence the course and outcome, but a positive disease outcome is not necessary for a family to feel successful. This flexible view of mastery permits the quality of relations within the family, or between the family and health care team, to become a central criterion of success. Health care providers’ competence is valued from both a technical and caregiving perspective, not solely from the biological disease course.
Families with the strongest and most rigid beliefs about control and personal responsibility may adapt well during earlier illness phases but become vulnerable if the condition progresses and beyond their control. A mind-set of “We understand the risks, and we are going to try our best to beat this cancer” promotes resilience, while “We must beat cancer or we’ve failed” fuels a feeling of defeat.
Fit Among Health Care Provider, Health Care System, and Family Beliefs
The same questions asked of families concerning beliefs are relevant to each of us on the health care team:
1.
What key values and health beliefs guide you in life? Clinicians also need to consider their own experiences and feelings about illness and loss (McDaniel et al., 1997; Rolland, 2018). Awareness and ease with our own multigenerational family history with illness and loss, our health beliefs, and our current developmental phase will enhance our ability to work effectively with families facing serious illness.
2.
What professional discipline and health care setting values guide you as a clinician?
3.
What are your views about both yours and the family’s ability to influence the illness course and outcome?
4.
How do you envision the balance between your and the family’s involvement in the treatment process? How can core belief differences be bridged?
Commonly, belief differences among family members or with the health care team emerge at major treatment or illness transition points. By example, in situations of severe disability or terminal illness, one family member may want the patient to return home, whereas another prefers transfer to an extended care facility. Because the primary caregiver role is typically assigned to the wife/mother, she is the one apt to bear most burdens in this regard. Anticipating the collision of gender-based beliefs about caregiving with the potentially overwhelming demands of home-based care for a severely disabled family member can help families flexibly modify their rules and avert the risk of family caretaker overload, resentment, and deteriorating family relationships.
The murky boundary between the chronic and terminal phase highlights the potential for providers’ beliefs to collide with those of the patient and family. Families may not know how to interpret continued life-saving efforts, assuming real hope where virtually none exists. Clinicians can feel governed by a technological obligation that requires them to exhaust all available treatments, regardless of the odds of success. The health care team can have its own difficulties stopping treatment. Continued treatment inertia can represent the health care team’s difficulty separating a core belief in controlling diseases from their beliefs about involvement (distinct from cure) in a patient’s total care, which includes bio-psycho-social-spiritual wellbeing.
Conclusion
Living well with the strains and uncertainties of illness can be a monumental challenge. The FSI Model offers a way to address this challenge and makes the inevitable strains more manageable. Attention to the psychosocial demands of different kinds of conditions over time within a multigenerational, developmental, and belief system context can help provide a strength-based framework—a common language that facilitates collaborative, creative problem-solving, and quality of life for families facing illness and disability.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
ORCID iD
John S. Rolland https://orcid.org/0009-0002-9386-6163
References
Berry E., Davies M., Dempster M. (2017). Exploring the effectiveness of couples interventions for adults living with a chronic physical illness: A systematic review. Patient Education and Counseling, 100(7), 1287–1303. https://doi.org/10.1016/j.pec.2017.02.015
Boersma P., Black L. I., Ward B. W. (2020). Prevalence of multiple chronic conditions among US adults, 2018. Preventing Chronic Disease, 17, E106. https://doi.org/10.5888/pcd17.200130
Boss P. (2011). Loving someone who has dementia: How to find hope while coping with stress and grief. Jossey-Bass.
Bowen M. (2004). Family reaction to death. In Walsh F., McGoldrick M. (Eds.), Living beyond loss: Death in the family (pp. 47–60). W. W. Norton.
Campbell T. L. (2003). The effectiveness of family interventions for physical disorders. Journal of Marital and Family Therapy, 29(2), 263–281. https://doi.org/10.1111/j.1752-0606.2003.tb01204.x
Carr A., Finneran L., Boyd C., Shirey C., Canning C., Stafford O.,. . .Burke T. (2024). The evidence-base for positive psychology interventions: A mega-analysis of meta-analyses. The Journal of Positive Psychology, 19(2), 191–205. https://doi.org/10.1080/17439760.2023.2168564
D’Onofrio B. M., Lahey B. B. (2010). Biosocial influences on the family: A decade review. Journal of Marriage and Family, 72(3), 762–782. https://doi.org/10.1111/j.1741-3737.2010.00729.x
Falicov C. J. (2015). Latino families in therapy: A guide to multicultural practice (2nd ed.). Guilford Press.
Franks H. M., Roesch S. C. (2006). Appraisals and coping in people living with cancer: A meta-analysis. Psycho-oncology, 15(12), 1027–1037. https://doi.org/10.1002/pon.1043
Gilliss C. L., Pan W., Davis L. L. (2019). Family involvement in adult chronic disease care: Reviewing the systematic reviews. Journal of Family Nursing, 25(1), 3–27. https://doi.org/10.1177/1074840718822365
Hansson K., Cederblad M. (2004). Sense of coherence as a meta-theory for salutogenic family therapy. Journal of Family Psychotherapy, 15(1–2), 39–54. https://doi.org/10.1300/j085v15n01_04
Hartmann M., Bäzner E., Wild B., Eisler I., Herzog W. (2010). Effects of interventions involving the family in the treatment of adult patients with chronic physical diseases: A meta-analysis. Psychotherapy and Psychosomatics, 79(3), 136–148. https://doi.org/10.1159/000286958
Kabat-Zinn J. (2023). Wherever you go, there you are: Mindfulness meditation in everyday life. Hachette.
Kazak A. E. (2006). Pediatric Psychosocial Preventative Health Model (PPPHM): Research, practice and collaboration in pediatric family systems medicine. Families, Systems & Health, 24(4), 381–395. https://doi.org/10.1037/1091-7527.24.4.381
Kirmayer L. J., Guzder J., Rousseau C. (Eds.). (2015). Cultural consultation: Encountering the other in mental health care. Springer.
Kleinman A. (2020). The illness narratives: Suffering, healing, & the human condition. Basic Books.
Knafl K. A., Deatrick J. A., Gallo A. M., Skelton B. (2021). Tracing the use of the family management framework and measure: A scoping review. Journal of Family Nursing, 27(2), 87–106. https://doi.org/10.1177/1074840721994331
Koenig H. (2012). Religion, spirituality, & health: The research and clinical implications. International Scholarly Research Notices Psychiatry, 2012, 278730. https://doi.org/10.5402/2012/278730
Lamson A. L., Hodgson J. L., Pratt K. J., Mendenhall T. J., Wong A. G., Sesemann E. M.,. . .Martin M. P. (2022). Couple and family interventions for high mortality health conditions: A strategic review (2010–2019). Journal of Marital and Family Therapy, 48(1), 307–345. https://doi.org/10.1111/jmft.12564
Lerner R. M. (2018). Concepts and theories of human development. Routledge.
Levinson D. J. (1986). A conception of adult development. American Psychologist, 41(1), 3–13. https://doi.org/10.1037/0003-066X.41.1.3
Martire L. M., Schulz R., Helgeson V. S., Small B. J., Saghafi E. M. (2010). Review and meta-analysis of couple-oriented interventions for chronic illness. Annals of Behavioral Medicine, 40(3), 325–342. https://doi.org/10.1007/s12160-010-9216-2
McDaniel S. H., Campbell T., Hepworth J., Lorenz A. (2013). Basic premises of family oriented primary care. https://link.springer.com/chapter/10.1007/0-387-26310-1_1
McDaniel S. H., Doherty W. J., Hepworth J. (2014). Medical family therapy and integrated care (2nd ed.). https://doi.org/10.1037/14256-000
McDaniel S. H., Hepworth J., Doherty W. J. (Eds.). (1997). The shared experience of illness: Stories of patients, families, and their therapists. Basic Books.
McGoldrick M., Carter B., Garcia Preto N. (Eds.). (2016). The expanded family life cycle: Individual, family and social perspectives (5th ed.). Pearson.
McGoldrick M., Gerson R., Petry S. (2020). Genograms: Assessment and intervention (4th ed.). W. W. Norton.
Miller S. M., McDaniel S. H., Rolland J. S., Feetham S. L. (Eds.). (2006). Individuals, families, and the new era of genetics: Biopsychosocial perspectives. W. W. Norton.
Peek C. J. (2015). Don Bloch’s vision for collaborative family health care: Progress and next steps. Families, Systems, & Health, 33(2), 86–98. https://doi.org/10.1037/fsh0000128
Proulx C. M., Snyder L. A. (2009). Families and health: An empirical resource guide for researchers and practitioners. Family Relations, 58(4), 489–504. https://doi.org/10.1111/j.1741-3729.2009.00568.x
Roesch S. C., Weiner B. (2001). A meta-analytic review of coping with illness: Do causal attributions matter. Journal of Psychosomatic Research, 50(4), 205–219. https://doi.org/10.1016/s0022-3999(01)00188-x
Rolland J. S. (1987). Chronic illness and the life cycle: A conceptual framework. Family Process, 26(2), 203–222. https://doi.org/10.1111/j.1545-5300.1987.00203.x
Rolland J. S. (1990). Anticipatory loss: A family systems developmental framework. Family Process, 29(3), 229–244. https://doi.org/10.1111/j.1545-5300.1990.00229.x
Rolland J. S. (1994a). Families, illness, and disability: An integrative treatment model. Basic Books.
Rolland J. S. (1994b). In sickness and in health: The impact of illness on couples’ relationships. Journal of Marital and Family Therapy, 20(4), 327–349. https://doi.org/10.1111/j.1752-0606.1994.tb00125.x
Rolland J. S. (1997). The meaning of disability and suffering: Sociopolitical and ethical concerns [Commentary]. Family Process, 36(4), 437–440. https://doi.org/10.1111/j.1545-5300.1997.00437.x
Rolland J. S. (2006a). Genetics, family systems, and multicultural influences. Families, Systems, & Health, 24(4), 425–442. https://doi.org/10.1037/10917527.24.4.425
Rolland J. S. (2006b). Living with anticipatory loss in the new era of genetics: A life cycle perspective. In Miller S., McDaniel S., Rolland J., Feetham S. (Eds.), Individuals, families, and the new era of genetics: Biopsychosocial perspectives (pp. 139–172). W. W. Norton.
Rolland J. S. (2016). Chronic illness and the life cycle. In McGoldrick M., Garcia N., Preto Carter B. (Eds.), The expanded family life cycle: Individual, family, and social perspectives (5th ed., pp. 430–454). Pearson.
Rolland J. S. (2017). Neurocognitive impairment: Addressing couple and family challenges. Family Process, 56(4), 799–818. https://doi.org/10.1111/famp.12316
Rolland J. S. (2018). Helping couples and families navigate illness and disability: An integrative approach. Guilford Press.
Rolland J. S., Emanuel L., Torke A. (2017). Applying a family systems lens to proxy decision making in clinical practice and research. Families, Systems, & Health, 35(1), 7–17. https://doi.org/10.1037/fsh0000250
Rolland J. S., Williams J. K. (2005). Toward a biopsychosocial model for 21st century genetics. Family Process, 44(1), 3–24. https://doi.org/10.1111/j.1545-5300.2005.00039.x
Ruddy N. B., McDaniel S. H. (2024). The developing evidence base for systemic interventions. In Ruddy N. B., McDaniel S. H. (Eds.), A systemic approach to behavioral healthcare integration: Context matters (pp. 181–194). American Psychological Association. https://doi.org/10.1037/0000381-009
Shields C. G., Finley M. A., Chawla N., Meadors P. (2012). Couple and family interventions in health problems. Journal of Marital and Family Therapy, 38(1), 265–280. https://doi.org/10.1111/j.1752-0606.2011.00269.x
Sousa H., Ribeiro O., Afreixo V., Costa E., Paul C., Ribeiro F., Figueiredo D. (2021). “Should WE Stand Together?”: A systematic review and meta-analysis of the effectiveness of family-based interventions for adults with chronic physical diseases. Family Process, 4, 1098–1116. https://doi.org/10.1111/famp.12707
Talen M. R., Burke A. B. (Eds.). (2013). Integrated behavioral health in primary care: Evaluating the evidence, identifying the essentials. Springer. https://doi.org/10.1007/978-1-4614-6889-9
Umberson D., Thomeer M. B. (2020). Family matters: Research on family ties and health, 2010-2020. Journal of Marriage and Family, 82(1), 404–419. https://doi.org/10.1111/jomf.12640
Walsh F. (Ed.). (2010). Spiritual resources in family therapy (2nd ed.). Guilford Press.
Walsh F. (Ed.). (2012). Normal family processes (4th ed., pp. 3–27). Guilford Press.
Walsh F. (2016). Strengthening family resilience (3rd ed.). Guilford Press.
Walsh F. (2023). Complex and traumatic loss: Fostering healing and resilience. Guilford Press.
Walsh F., McGoldrick M. (2013). Bereavement: A family life cycle perspective. Family Science, 4(1), 20–27. https://doi.org/10.1080/19424620.2013.819228
Weihs K., Fisher L., Baird M. (2002). Families, health, and behavior: A section of the commissioned report by the Committee on Health and Behavior: Research, Practice and Policy Division of Neuroscience and Behavioral Health and Division of Health Promotion and Disease Prevention Institute of Medicine, National Academy of Sciences. Families, Systems, & Health, 20(1), 7–46. https://doi.org/10.1037/h0089481
Wood B. L., Woods S. B., Sengupta S., Nair T. (2021). The Biobehavioral Family Model: An evidence-based approach to biopsychosocial research, residency training, and patient care. Frontiers in Psychiatry, 12, Article 725045. https://doi.org/10.3389/fpsyt.2021
Wright L. M. (2017). Suffering and spirituality: The path to illness healing. 4th Floor Press.
Wright L. M., Bell J. M. (2009). Beliefs and illness: A model for healing. 4th Floor Press.
Wright L. M., Bell J. M. (2021). Illness beliefs: The heart of healing in families and individuals (Revised 3rd ed.). 4th Floor Press.
Biographies
John S. Rolland, MD, MPH is Professor of Psychiatry at Northwestern University Feinberg School of Medicine and Co-Founder and Executive Co-Director, Chicago Center for Family Health. Widely recognized for his conceptual model and clinical work with couples and families facing serious health conditions, his recent book is Helping Couples and Families Navigate Illness and Disability: An Integrated Approach. Other professional books include his landmark volume, Families, Illness, & Disability: An Integrative Treatment Model; and (co-author) Individuals, Families and the New Era of Genetics. He is a Distinguished Life Fellow of the APA, past President of the American Family Therapy Academy (AFTA), and recipient of numerous professional awards.
Cite
Cite
Cite
OR
Download to reference manager
If you have citation software installed, you can download citation data to the citation manager of your choice
Information, rights and permissions
Information
Published In
Article first published online: April 12, 2025
Issue published: May 2025
Keywords
Article versions
You are viewing the most recent version of this article. To download and view previous versions, see below:
PubMed: 40219674
Authors
Metrics and citations
Metrics
Publication usage*
Total views and downloads: 3767
*Publication usage tracking started in December 2016
Publications citing this one
Receive email alerts when this publication is cited
Web of Science: 3 view articles Opens in new tab
Crossref: 3
- Realization of a Family Systems Care Unit: A Real-Life Laboratory for Clinical Practice, Education, and Research at a Swiss University of Applied Sciences
- The Key to Child Independence Starting at Home: A Case Study on The Role of Parenting Styles and Practical Life Skills
- Through mothers’ eyes: A qualitative exploration of raising a child with cystic fibrosis
Figures and tables
Figures & Media
Tables
View Options
View options
PDF/EPUB
View PDF/EPUBAccess options
If you have access to journal content via a personal subscription, university, library, employer or society, select from the options below:
loading institutional access options
Alternatively, view purchase options below:
Purchase 24 hour online access to view and download content.
Access journal content via a DeepDyve subscription or find out more about this option.




