Background
More than 11 million adults in the U.S. provide unpaid care to family members, friends, and other people living with Alzheimer’s disease and other dementias (ADRD).
1 ADRD caregivers are particularly susceptible to physical, social, emotional, and financial challenges, more so than caregivers of older individuals living with other chronic conditions, given the extensive assistance they tend to provide.
2 Beyond the nature of tasks being provided during care, caregiving experiences can vary depending on additional factors such as caregiving duration and the social position of the caregiver (e.g., race/ethnicity, sexual orientation, gender identity), factors that ultimately influence the caregiver’s health and well-being.
1,3LGBTQ+ is an umbrella term used to describe people who self-identify as lesbian, gay, bisexual, transgender, queer, nonbinary, intersex, and/or who express behaviors and attractions that do not align with heterosexual or conventional gender norms.
4 Recent population-based data estimates suggest that 1 in 5 LGBTQ+ adults are caregivers to a family member or friend with a disability or health problem. Over half of these caregivers are providing personal care (e.g., medical/nursing tasks) and approximately 20% are providing care to someone living with ADRD.
5 Research about LGBTQ+ ADRD caregivers is limited; however, LGBTQ+ ADRD caregivers have reported fewer financial and social resources and caregiver supports than non-LGBTQ+ ADRD caregivers and may be caring for someone who does not accept their LGBTQ+ identity, which can increase the psychological impact of caregiving.
6 In fact, findings from a study with a convenience sample of only LGBTQ+ ADRD caregivers found the majority of the sample reported elevated depressive symptoms and below average health.
3 Bi+ populations, those with non-monosexual identities (e.g., bisexual, pansexual, queer), are the largest sexually minoritized group in the U.S, and research suggests they face significant health disparities compared with both monosexual minority (i.e., gay, lesbian) and heterosexual individuals.
7-9Research suggests that disparities in health and well-being among bi+ individuals may be understood within an expanded Minority Stress and Resilience Framework.
10 Within the Minority Stress Framework,
11 health disparities among sexual minority populations arise from chronic exposure to stigma, discrimination, and social marginalization, as well as the expectation of these stressful experiences. Feinstein and Dyar
10 further expanded the Minority Stress Framework to theorize the phenomenon of bisexual-specific stressors, such as monosexism, identity invalidation, and erasure within both monosexual minority and heterosexual communities, factors that can lead to social isolation, invisibility, internalized stigma and consequently, poorer health outcomes. For some, the ability to “pass” as heterosexual may temporarily buffer exposure to external stigma, but it can also reinforce invisibility, erode identity affirmation, and reduce opportunities for social support. While such challenges can threaten the health of bi+ individuals,
12-15 protective factors such as identity integration, affirming social networks, and community connectedness can mitigate these stressors by fostering resilience and psychological well-being.
11,16,17 Identity integration promotes self-acceptance and reduces internalized stigma, buffering the emotional strain associated with identity concealment or invalidation.
11,17 Affirming social networks provide validation and emotional support, directly counteracting experiences of rejection and isolation, while community connectedness enhances belonging and access to collective coping resources.
18,19The combination of minority stress and the demands of ADRD caregiving likely influence the health and well-being of bi+ caregivers. The unique stressors that many bi+ individuals experience (e.g., monosexism, isolation), can intersect with ADRD caregiving challenges (e.g., burnout, limited respite), amplifying vulnerability to caregiver burden and poor mental health.
20,21 Bi+ caregivers may have reduced access to bi+- affirming caregiver support groups both within and outside of the LGBTQ+ community or experience invisibility within mainstream aging and ADRD networks.
22 Without affirming spaces to share their experiences, bi+ caregivers may internalize stigma or conceal their identity, further intensifying poor mental health outcomes. Conversely, when bi+ identities are affirmed and they are included within both LGBTQIA+ and caregiving communities, minority stress can be buffered, creating opportunities for resilience, coping capacity, psychological well-being, and caregiving engagement.
10,19Despite comprising the largest segment of the sexual minority population and experiencing unique stressors and health disparities, bi+ ADRD caregivers remain underrepresented in health and caregiving research and have been described as the
invisible majority.
9 Furthermore, ADRD caregivers have been characterized as
invisible second patients23 due to the substantial physical, emotional, and social demands of ADRD caregiving. Taken together, these dual forms of invisibility suggest that we can appropriately consider bi+ ADRD caregivers as a
twice hidden population. Given that existing research suggests that both ADRD caregiving challenges and minority stress can influence health, the current study examined associations between minority stress and stress on global health to determine if these associations differed among bi+ and gay/lesbian (g/l; monosexual) ADRD caregivers. We hypothesized that both minority and caregiving stress would be negatively associated with global health and that the impact would be greater for bi+ caregivers than g/l caregivers.
Discussion
This study contributes to the growing body of literature highlighting the heterogeneity of LGBTQ+ caregivers by demonstrating meaningful differences between bi+ and g/l ADRD caregivers across sociodemographic characteristics, minority and caregiving stressors, and global health. These findings reinforce the importance of examining differences in caregiving and health outcomes at the level of specific sexual minority subgroups rather than treating LGBTQ+ caregivers as a monolithic group. Notably, this study addresses a significant gap in the literature by centering bi+ ADRD caregivers, who are underrepresented in health research. Our results indicate that for bi+ caregivers, their experiences of stress, caregiving, and health differ in important ways from those of g/l caregivers, underscoring the need for more thoughtful approaches to caregiving supports, services, and future research that address the specific needs of each sexual minority subgroup.
Caring for a spouse or partner was the most common relationship type among both groups, though this was more frequent among g/l caregivers (61.5%) than bi+ caregivers (35.2%). This difference may be partially explained by limitations in the measure used to assess the caregiver–care recipient relationship, particularly regarding how spousal or partner categories were defined. The measure may not have fully captured relationship configurations more commonly reported among bi+ individuals, such as those identifying as pansexual or omnisexual.
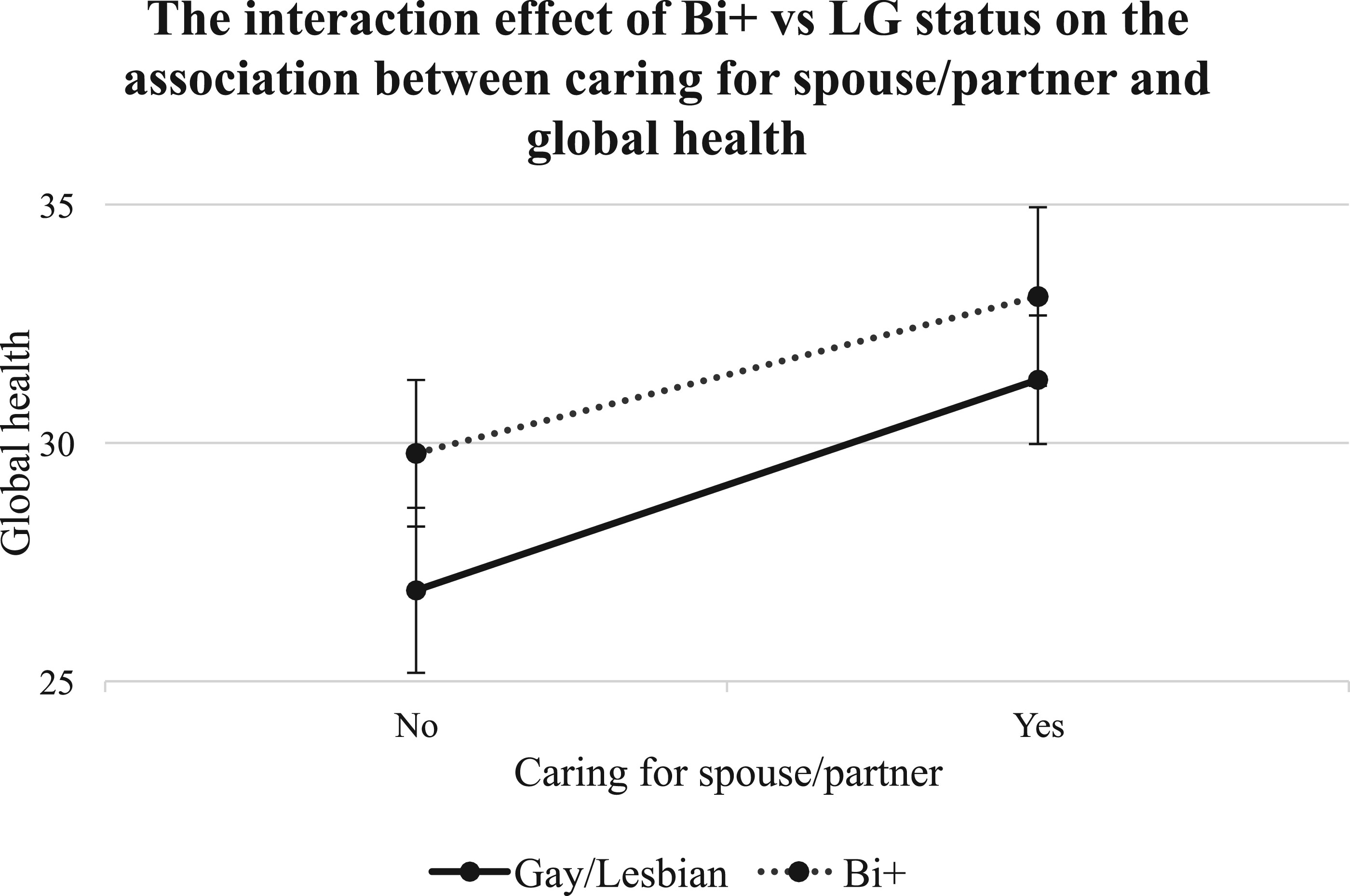
In contrast to expectations, caring for a spouse or partner was positively associated with global health in adjusted models. This finding may reflect the well-established protective effects of a close and supportive marriage and partnership on health, including greater emotional support, social integration, and access to shared resources, rather than caregiving stress alone. Because marital or partnership status was not included as a separate covariate, and the original study did not assess relationship quality, it is possible that the spouse/partner caregiving variable captures both caregiving role and relational context. Future studies should distinguish caregiving relationship type from marital or partnership status and assess relationship quality to better disentangle caregiving burden from the health-promoting effects of supportive intimate partnerships.
Additionally, the gender of the caregiver’s partner was not collected and was not considered in the validated measures utilized. As such, it is plausible that bi+ caregivers who were married or partnered may have experienced differential levels of minority stress depending on whether others perceived their relationship as heteronormative or as indicative of LGBTQ+ identity.
35LGBTQ+ individuals are recognized as a health-disparate population, with a substantial body of research indicating these disparities are often driven by minority stress, including experiences of discrimination related to their LGBTQ+ identities.
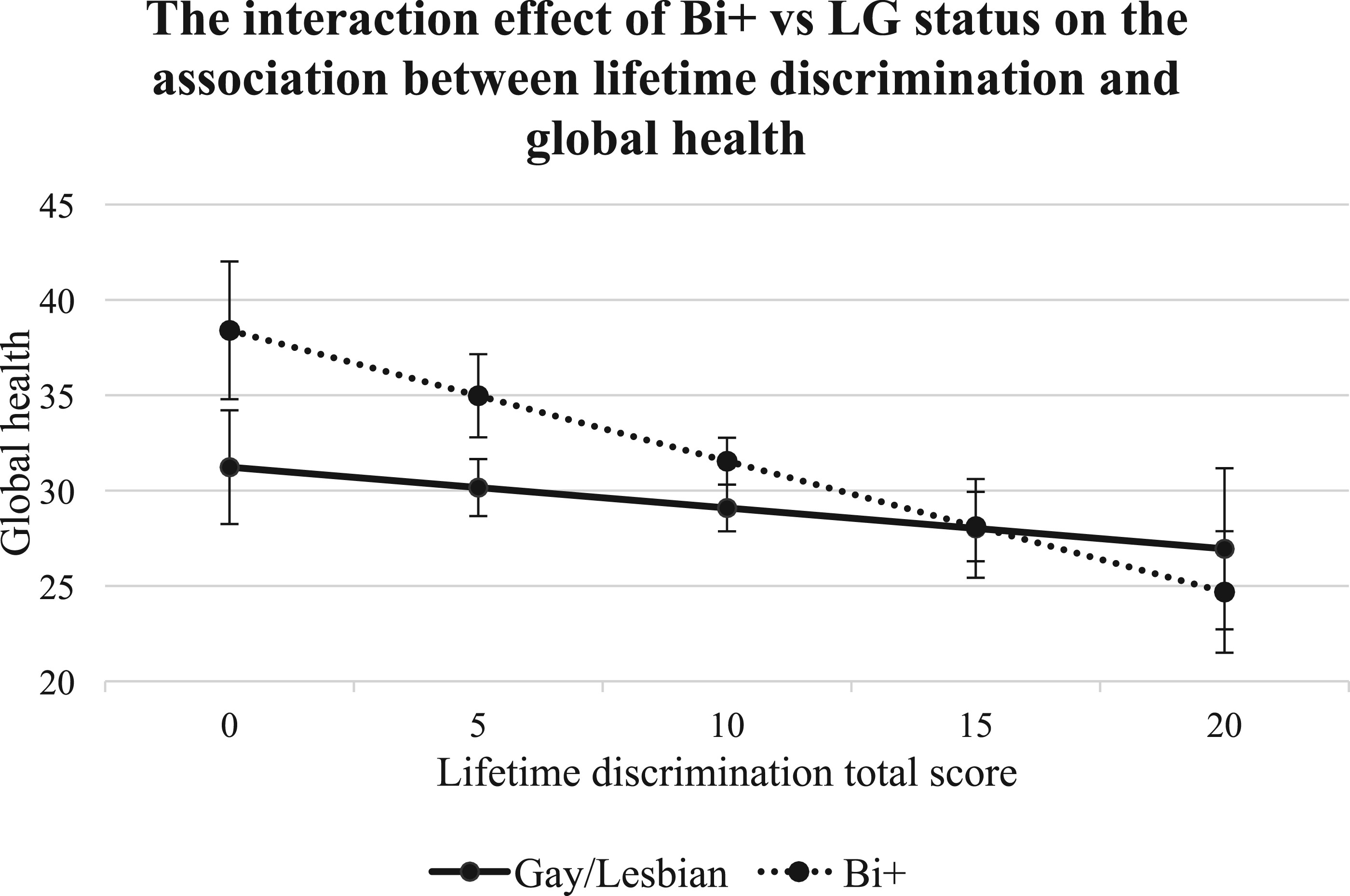
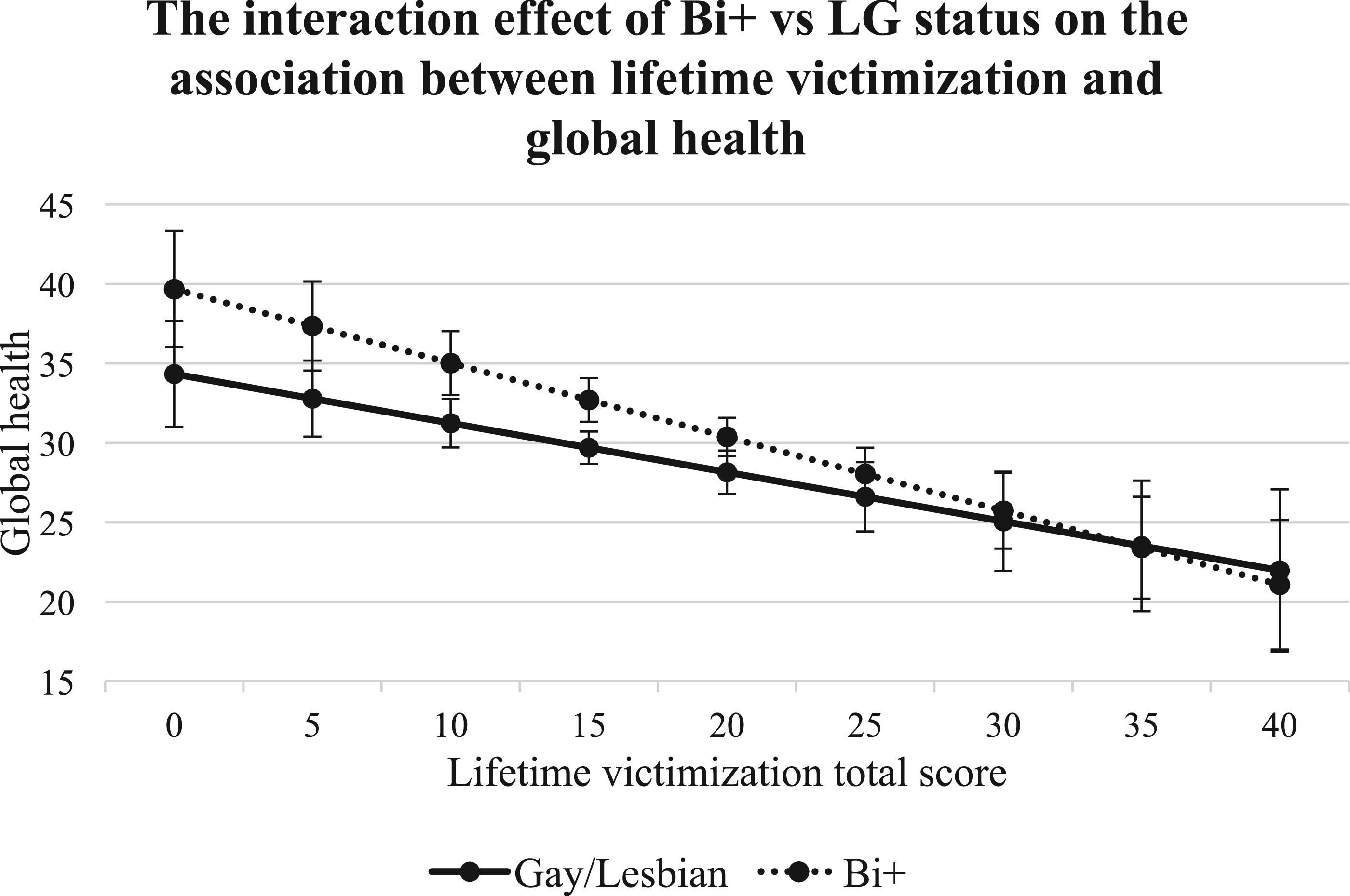
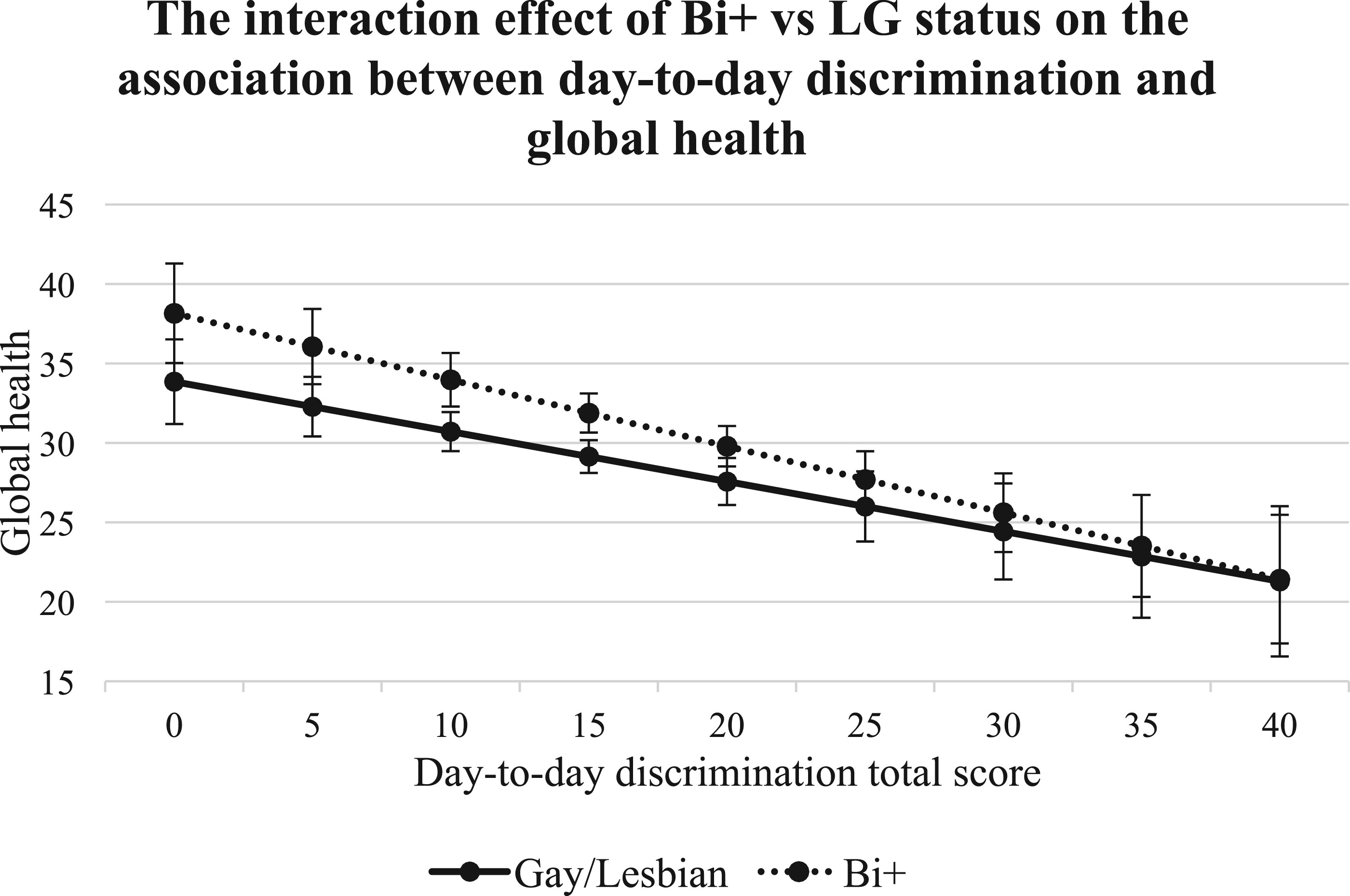
7-9,11,12 In line with this evidence, the present study found that lifetime discrimination, lifetime victimization, daily discrimination, and microaggressions were negatively associated with global health among both bi+ and g/l ADRD caregivers. Notably, higher lifetime discrimination scores predicted poorer global health for both groups, with the magnitude of this association being stronger for bi+ caregivers compared with g/l caregivers. These findings underscore the existence of health disparities within the bi+ caregiver population and highlight the presence of bi+-specific minority stress, at least in terms of lifetime discrimination, on global health. These results are consistent with minority stress theory,
11 which posits that chronic exposure to discrimination and stigma accumulates over the life course, negatively affecting mental and physical health. This cumulative stress may be particularly pronounced among bi+ caregivers, who have been shown to lack the buffering effects of LGBTQ+ community support that can mitigate minority stress and promote well-being among g/l caregivers.
36An expanded minority stress framework
10 provides a useful framework for understanding the unique stressors experienced by bi+ individuals due to anti-bisexual stigma, which differ from those experienced by their monosexual counterparts. Bi+ caregivers in our sample experienced more minority stress than g/l caregivers, including higher levels of victimization. Higher levels of victimization among bisexual people compared with lesbian and gay individuals have been found in previous research.
15 These elevated levels of minority stress may reflect the compounded negative attitudes bi+ individuals receive from heterosexual people because of their nonconformity to heteronormative standards, as well as from lesbian and gay people because of their nonconformity to monosexual standards.
35 Binegativity and hostility stemming from pervasive stereotypes that bisexuality is unstable, illegitimate, or inherently promiscuous can significantly undermine the ability of bisexual individuals to access safe and supportive communities. These stigmatizing beliefs not only contribute to social exclusion but also have deeply personal consequences. For example, stereotypes surrounding bi+ promiscuity and the perceived illegitimacy of bisexual identities can adversely affect romantic opportunities. Empirical research has shown that such negative attitudes often manifest in reluctance among heterosexual, gay, and lesbian individuals to engage in romantic relationships with bisexual partners.
10 Additionally, bi+ identities are questioned or invalidated when individuals are in monogamous relationships due to the erroneous assumption that bisexuality requires simultaneous involvement with partners of multiple genders to be legitimate.
37 Importantly, community belonging and being in romantic relationships have shown to be protective factors of health that can even mitigate the harms of minority stress.
9,36,38,39The degree to which an individual is perceived by others as belonging to an LGBTQ+ group may influence the experience of minority and caregiving stress. Research has demonstrated that perceived LGBTQ+ status can increase exposure to minority stressors. Bisexual individuals are more likely to experience stress related to disclosing and/or concealing their sexual identities than their g/l peers to avoid bi-negativity, limiting potential positive opportunities for connection with LGBTQ+ communities and reducing access to protective social support networks.
10,16,19 Furthermore, among bi+ individuals in romantic partnerships, perceptions of their LGBTQ+ identity are often shaped by the gender of their partner, especially within monogamous relationships. For example, bisexual women partnered with other women are frequently assumed to be lesbians, even when they explicitly disclose a bisexual identity. Such misperceptions are associated with sexual identity questioning and uncertainty, where individuals begin to doubt whether the label ‘bisexual’ accurately reflects their sexual identity.
35 Moreover, there is evidence that bisexual women with male partners report more frequent experiences of bi-negativity compared with those with female partners, and this increased bi-negativity is linked to heightened levels of depression and alcohol use problems.
35,40 Qualitative studies further indicate that bisexual identity erasure and feelings of invisibility in monogamous relationships are experienced as stressful and are associated with adverse mental health outcomes.
41Bi+ caregivers in this study also had significantly lower family quality life scores. It is reasonable that the bi+ caregivers in our sample, who are experiencing more minority stress while also caring for someone with ADRD, may also be struggling with the quality of their family life and caregiving may be adding strain to their family. Income is another potential contributing factor, as many of the questions on the FQOLDS are influenced by income and other research has found a positive association between income and higher family quality of life scores among gay men.
42 However, it is imperative to note that the FQOLDS was not developed to capture the unique experiences of family life for LGBTQ+ caregivers. The FQOLDS does not account for LGBTQ+ individuals caring for a parent who is not accepting or affirming of their identity. This is a critical omission, as LGBTQ+ individuals who care for a parent report experiencing three times more emotional strain than their non-LGBTQ+ counterparts.
22 Additionally, the FQOLDS assumes the LGBTQ+ caregiver is caring for their family member living with ADRD. This may be problematic as research shows that LGBTQ+ caregiving often occurs between friends not just among family
38 and the bi+ caregivers in our study were less likely to be caring for their spouse or partner. The LGBTQ+ population is known for having non-traditional family structures due to experiencing stigma and discrimination from their birth family members, such as family rejection. As a result, LGBTQ+ people often create what is known as a chosen family, or a group of individuals who are not members of their birth family, who provide love and support, and this aspect of family is not addressed by the FQOLDS. Our understanding of LGBTQ+ caregivers family experiences with ADRD would benefit from further research that captures the lived experiences of LGBTQ+ caregivers with more accuracy, including bi+ caregivers whose family structures might look quite different than heterosexual and g/l caregivers.
For both bi+ and g/l caregivers, higher family quality of life scores predicted better global health, although the magnitude of this association was stronger for bi+ caregivers compared with g/l caregivers. It could be that family quality of life among bi+ caregivers may transcend the other challenges in their lives, which might include experiences of minority stress, bringing the most meaning to their lives and, ultimately, have a positive impact on their global health. Nevertheless, the lack of consideration of the lived experiences of LGBTQ+ ADRD caregivers in the FQOLDS previously mentioned likely discounts our opportunity to more accurately understand the influence of family quality of life in the caregiving experiences and health of bi+ and gay/lesbian ADRD caregivers.
Bi+ caregivers in this study reported higher global health scores than g/l caregivers. Research consistently demonstrates that bi+ people experience significant mental health disparities compared with their monosexual g/l and heterosexual counterparts,
9,12-15 but less is known about the physical health disparities between these groups. While some research notes a higher risk of cardiovascular disease
43 and obesity
44 among bisexual and lesbian women compared with heterosexual women, physical health differences among sexual minority subgroups are understudied. Our finding of bi+ caregivers reporting better health than g/l caregivers differs from what was found in a study
21 that examined health-related quality of life among lesbian and bisexual women, which found a higher likelihood of poor general health among bisexual women than lesbians. Additionally, the higher global health scores observed among bi+ caregivers may, in part, be attributed to the proportion of individuals in this group caring for a spouse or partner, compared with g/l caregivers, as previous studies suggest that spousal and partner caregivers often experience poorer physical and mental health outcomes than non-spouses/partners.
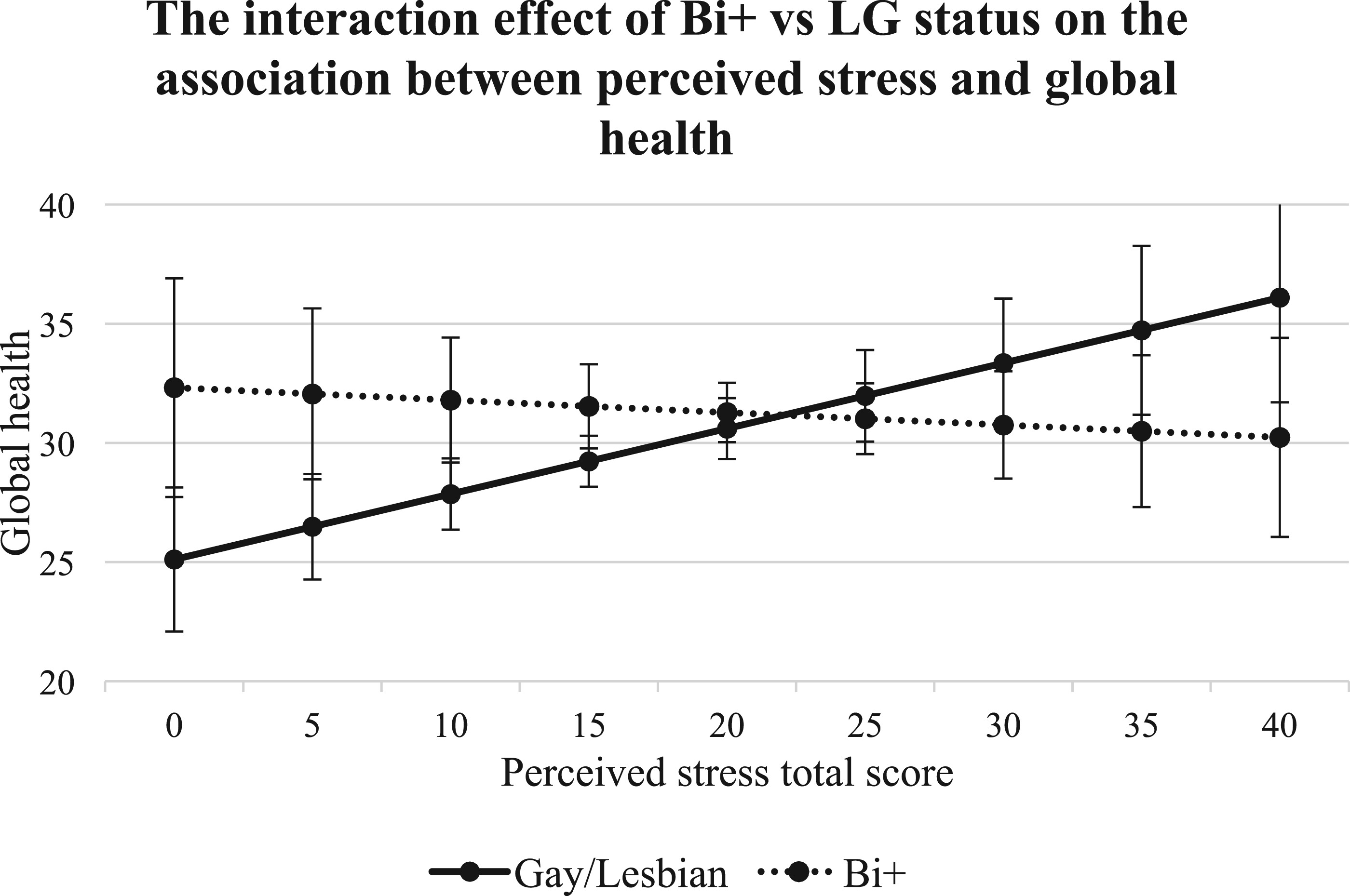
21Unexpectedly, we found that perceived stress was positively associated with global health and this association differed between bi+ and g/l caregivers. Higher perceived stress scores predicted worse global health for bi+ caregivers, yet higher perceived stress scores predicted better global health for g/l caregivers. While we did not examine social connection in the current study, one possible explanation for this finding could be related to differences in social connection between the two groups. For example, g/l caregivers in our sample who report high levels of stress may turn to LGBTQ+ community-serving organizations for support and social engagement. Programs offered by LGBTQ+ community-serving organizations are often tailored to g/l individuals, with limited offerings specifically designed for bi+ community members.
45 These types of supportive services and connection with other LGBTQ+ community members are protective and can help mitigate the negative effects of stress on health.
35 It is possible that the bi+ caregivers in our sample who are experiencing high levels of stress may have less access to LGBTQ+ community connections and, therefore, may not be reaping the potential protective reward of such engagement, a disparity suggested in previous studies.
35,36,39There are important research and practice implications that should be considered based on our findings. At the time of writing, research funding for LGBTQ+ health in the U.S. is under threat, posing a significant barrier to advancing knowledge about bi+ individuals, including those providing care to persons living with ADRD.
46 Researchers must continue to identify ways to conduct research, which includes data collection efforts that incorporate inclusive measures that are able to capture the diverse experiences of all LGBTQ+ subgroups at a time when public health infrastructure supporting such efforts is being abrogated. Continuing LGBTQ+ health research efforts is critical for informing best practices and developing evidence-based policies aimed at eliminating LGBTQ+ health disparities. Additional research is critically needed to develop new measures and adapt existing ones to accurately reflect the lived experiences of LGBTQ+ caregivers. Furthermore, it is imperative that practitioners working with bi+ populations, including those who are ADRD caregivers, are educated on the unique ways in which minority stress influences caregiving experiences and health. By fostering a safe and affirming environment, providers can more effectively support bi+ clients and patients. Moreover, providers should play an active role in advocating for inclusive practices and policies across the broader health care system and within community-based programming, including LGBTQ+ centers. It may be beneficial for LGBTQ+ community health centers to routinely assess the existence and effectiveness of their bi+-inclusive policies and programming, adjusting as needed to ensure bi+ individuals are included, supported, and represented.
Limitations
Given that we used a secondary analysis of existing data, our analysis was subject to certain limitations related to the data collected and measures used by the original study. As such, we were unable to assess the influence of LGBTQ+ community connection or the gender of the caregiver’s partner or spouse on the associations tested. Furthermore, the cross-sectional nature of the data limited our ability to examine how minority and caregiving stressors may change over time; therefore, we were unable to assess causality. Our sample of ADRD caregivers was restricted to individuals with internet access and the ability to navigate the online survey platform, which may preclude generalizability. Study materials were only available in English and therefore the results reflect the experiences of English-speaking caregivers only and may not be representative of non-English-speaking populations. Finally, our classification of bi+ participants was restricted to the only survey item that assessed sexual orientation, as there were no survey items that queried sexual attraction or behavior. Future research should employ multidimensional measures of sexual orientation (ie, identity, attraction, and behavior) to more comprehensively capture research participants who may not self-identify as one of the sexual orientation identities we used to conceptualize the bi+ caregivers study group. Despite these limitations, this study makes an important contribution to the literature by highlighting limitations in existing caregiving measures, many of which likely fall short in capturing the lived experiences of gay, lesbian, and bi+ ADRD caregivers and especially are lacking in attention to nuanced subgroup differences in measurement.