Non-pharmacological interventions feasible in the nursing scope of practice for pain relief in palliative care patients: a systematic review
Abstract
Background:
Objectives:
Design:
Data sources and methods:
Results:
Conclusion:
Trial registration:
Introduction
Methods
Protocol and registration
Literature search
Eligibility criteria
Study selection
Data extraction and study quality
Best-evidence synthesis
Results
Study selection
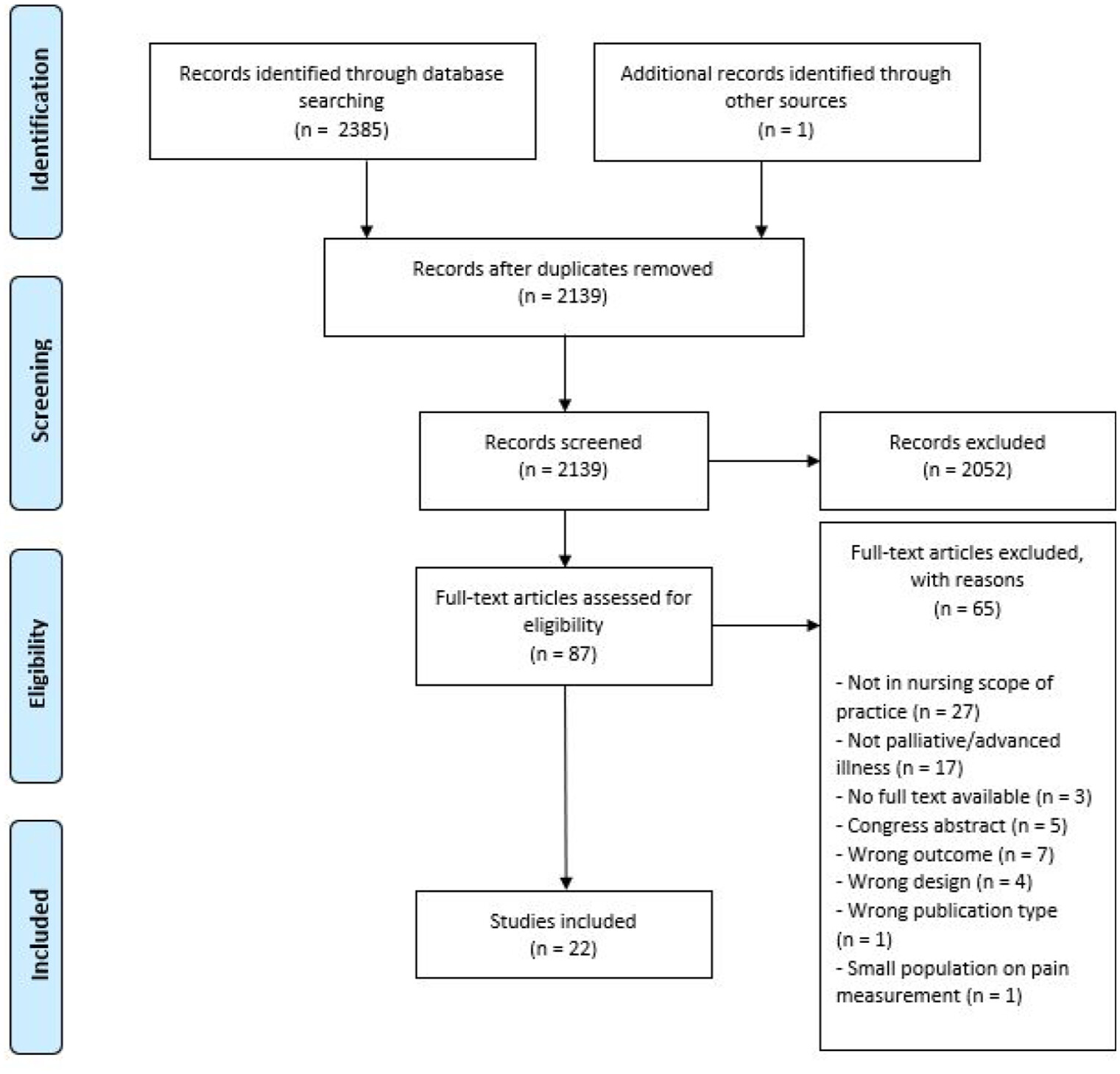
Data extraction and study quality
| References | Study design | Total participants + chronic/acute pain, characteristics mean ± SD, range, (n) and/or n (%) | Intervention(s) + professional performing the intervention during study | Data collection interval | Scale used | Data analysis (within/between groups) | Results (data of pain); mean ± SD |
|---|---|---|---|---|---|---|---|
| Mitchinson et al.21 2014 USA | Observational study | 153 veterans with advanced illnesses; Chronic/acute pain: 70% preexisting chronic pain Age 65.2 ± 12.2; Gender (male) 146; Primary cancer site (105): lung (31), head and neck (17), gastrointestinal (25), genitourinary (16), hematologic (6), other (10) Primary non-cancer diagnosis (48): COPD (10), End-stage renal disease (6), congestive heart failure (8), dementia (5), other (19) | 20–30 min massage: consisting of effleurage massage with some limited trigger point. Light to moderate pressure applied depending on patient’s health. Professional: hospice and palliative medicine fellow or a member of the palliative care consultation team | Pretreatment and posttreatment | 0–10 scale adapted from Well-Being Scale of Giasson 0 = no pain, 10 = severe pain | One-sided sign test Chi-square test | Mean change pain intensity 1.65 ± 2.14; Significantly decreased (p < 0.001) Chronic pain showed greater decrease in pain intensity compared to non-chronic pain patients Cancer patients showed greater decrease in pain intensity compared to non-cancer patients |
| Kutner et al.18 2008 United States | Randomized trial | 380 hospice patients with advanced cancer; Chronic/acute: not stated Intervention group (n = 188)/Control group (n = 192): Age 65.2 (14.4%)/64.2 (14.4%); Gender (female) 120 (64%)/112 (58%); Primary cancer site: lung (48/48), breast (34/29), pancreas (13/22), colorectal (12/17), prostate (10/11) | Massage group (n = 188): 6× 30-min massage light/gentle effleurage (smooth/gliding strokes), petrissage (squeezing, rolling, and kneading the muscles) and myofascial trigger point release (concentrated finger pressure to painful localized areas in muscles). Masseur judgment dictated rhythm/rate/stroke frequency, sequence/mix of strokes, time spent each stroke, stroke length, and body area massaged. Control group (simple touch): placement of both hands for 3 min at each of the following locations bilaterally: base of neck, shoulder blades, lower back, calves, heels, clavicles, lower arms, hands, patellae, and feet. Professional: massage therapist | Pretreatment and posttreatment for immediate effect Weekly follow-up for sustained effect | Immediate effect: MPAC (0–10); 10 = worst pain Sustained effect: BPI scales for worst pain, least pain, pain on the average, pain right now (0–10); 0 = no pain, 10 = pain as bad as you can imagine | T-test (continuous); Chi-square test (categorical) Sustained outcome: comparison average of three post-baseline means and baseline mean Immediate outcome: average across means (all six visits) | Immediate outcome; Massage group (n = 151): −1.87 points improvement (95% CI: −2.07, –1.67); Clinically significant Control group (n = 147): −0.97 (95% CI: −1.18, −0.76) Mean difference: −0.9 (95% CI: −1.19, −0.61); Approaches clinical significance Both groups (massage n = 171, control n = 177) demonstrated statically, but not clinically, significant sustained improvements in pain |
| Jane et al.22 2009 Taiwan | Quasi-experimental | 30 hospitalized cancer patients with bone metastases; Chronic/acute pain: not stated Age 51.7 ± 11.6; Gender (female): 19 (63%); Primary cancer site: lung (11), breast (11), head and neck (2), gastrointestinal (4) | 45-min of massage therapy: hands-on and skin-to-skin manipulation of soft tissue of highly innervated (i.e. head, hand, feet) and less innervated (i.e. back, limbs) regions Professional: registered nurse | Pretreatment, posttreatment, short-term (20–30 min follow-up), intermediate (1–2.5 h) and long-term (16–18 h) | PPI with a vertical form of VAS (0–100 mm); 0 = no pain, 100 = pain as bad as it could be | Paired t-test Repeated measures analysis of variance | Baseline: 5.4 ± 1.2; Immediate effect: 3.1 ± 1.4 (p = 0.000); Short-term effect: 2.8 ± 1.8 (p = 0.000); Intermediate effect: 3.2 ± 2.0 (p = 0.000); Long-term effect: 3.8 ± 2.0 (p = 0.000) Most significant impact occurred 15 (p < 0.002) or 20 (p < 0.000) minutes after the intervention |
| Wilkie et al.19 2000 USA | Randomized clinical trial (pilot) | 29 hospice patients; Chronic/acute pain: not stated Age 63 (3085); Gender (female): 21 (38%); Primary cancer site: lung (21%), breast (7%), prostate (7%), colorectal (10%), other (55%) | 30–45 min full-body massage twice weekly massage for 2 weeks; Following strokes delivered: effleurage, light petrissage, nerve stroke, light compression, vibration, tapotement (n = 15) Control: usual hospice care (n = 14); Professional: massage therapists | Pretreatment and posttreatment (before and after each of four massages) | Pain Assessment Tool or Skilled Nursing Visit Report form (0–10); 0 = no pain, 10 = worst ever | Paired t-test (within groups) Independent t-test (between groups) | Control: Baseline: 1.6 ± 2.1, Outcome: 1.2 ± 1.3 Massage: Baseline: 2.4 ± 2.8, Outcome: 1.5 ± 1.4 Between groups: Baseline: p > 0.43, Outcome: p > 0.73 |
| Pedersen et al. 23 2017 Sweden | Observational study | 41 patients at hospice ward; Chronic/acute pain: not stated Age 71 (38–95); Gender (female): 24 (59%); Primary diagnosis: advanced cancer (35), COPD (3), terminal heart failure (3) | Tactile massage: soft and superficial form of massage with slow strokes, light pressure and circling movement on the feet, hands, and/or back. Relaxing music played in the background for 15–45 min Professional: tactile masseuse | Pretreatment and posttreatment | ESAS (0–10); 0 = no pain, 10 = worst possible pain Rescue dose medication (opioids) 24 h before and after treatment | Paired t-test | Difference p < 0.0001 [Figure estimation] Pretreatment: 2.7, Posttreatment: 1.0 (n) of rescue doses Pretreatment: 1.8, Posttreatment: 0.8, p = 0.0005 Same patients 4 (control day 1) and 3 (control day 2) days before first treatment Control day 1: 1.8, Control day 2: 1.9, p = 0.20 |
| Havyer et al.20 2020 USA | Single-arm pilot study | 27 hospice patients; Chronic/acute pain: not stated Age: 77 (44–102); Gender (female): 10 (37%); Primary diagnosis: cancer 19 (70.4%), heart disease 2 (7.4%), pulmonary disease 1 (3.7%), dementia 1 (3.7%), renal disease 2 (7.4%), multisystem atrophy 1 (3.7%), parkinsonism 1 (3.7%) | Massage therapy (20–45 min sessions up to three sessions every 1–2 weeks) Professional: massage therapist | 72 h prior to and after each session and final assessment 1 week after final session | ESAS-r | Sign rank test | Median change (final measure − baseline measure): 0 (−6 − 7), p = 0.3787 |
| Soden et al.29 2004 United Kingdom | Randomized controlled trial | 42 cancer patients in hospice; Chronic/acute pain: not stated Age 73 (44–85); Gender (female) 32 (75%); Primary cancer site: breast (15), lung (8), gastrointestinal (4), head and neck (4), prostate (3), other (8) | Aromatherapy group: 30-min back massage with lavender essential oil and an inert carrier oil (sweet almond oil) to a dilution of 1% Massage group: massage with an inert carrier oil only Control group: no massage Professional: not stated | Pretreatment and posttreatment (4 h after) Baseline and after 4 weeks follow-up | VAS (0–10 cm); 0 = least possible pain, 10 = worst possible pain | Paired t-test ANOVA | Mean change baseline − final assessment: Aromatherapy 0.19 (p = 0.87), Massage 0.32 (p = 0.63), Combined massage 0.25 (p = 0.69), Control group 0.78 (p = 0.32) Statistically significant reduction in both aromatherapy (p = 0.03) and combined massage (p = 0.01) after the second treatment |
| Louis et al.30 2002 United States | Quasi-experimental | 17 in-home hospice patients; Chronic/acute pain: not stated Age 61.76 (42–79); Gender (female) 8 (47%); Terminal cancer 17 (100%) | 60 min of humidified inhalation of 3% essential lavender oil (Lavandula angustifolia). Three drops of essential oil mixed with 5 cc of water in an electric potpourri pot at 4 ft from the subject (for 60 min a total of 30 drops and 50 cc water was used) (n = 17, same group as control) Control group: no intervention (day 1) (n = 17); Humidified water intervention group (day 2) (same group as control) Professional: self-applied by patients | Pretreatment and posttreatment | NRS (0–10); 0 = no pain, 10 = highest level of unbearable, excruciating pain | Paired t-test | Control group: Pretest: 1.38, Posttest: 1.70 Water group: Pretest: 2.09, Posttest: 1.66 Lavender group: Pretest: 1.59, Posttest: 1.25 Not statistically significant within groups |
| Lee et al.32 2017 South Korea | Prospective interventional | 18 outpatients with metastatic breast cancer; Chronic/acute pain: not stated Intervention group/Control group: Age 52 (35–64)/57 (37–67); Median time diagnosis of metastasis and enrolment: 18 months; Metastatic lesion: Brain (1/1), lung (5/4), liver (4/3), bone (4/5), lymph nodes (4/6), anterior chest wall (3/3), skin (0/2), pleural effusion (1/0) | MBSR program: once a week, 2-h session for 8 weeks. Daily home practice with 54-min compact discs of mindfulness practices (n = 9) MBSR: body scan that concentrated on the body from head to toe to observe the sensations felt in each area, sitting meditation, some group discussions in which patients had time to share experiences, and mindfulness in communication and everyday life. Control group: usual care (n = 9) Professional: MBSR instructor | Pretreatment and posttreatment | Wisconsin Brief Pain Inventory. Pain intensity (0–10) | Wilcoxon signed-rank test | MBSR: Pretest: 3.44 ± 1.74, Posttest: 3.11 ± 2.09 Control group: Pretest: 1.78 ± 1.99, Posttest: 3.11 ± 2.57 Change was not statistically significant between groups (p = 0.080) |
| Guan et al.24 2021 Malaysia | Randomized controlled trial | 60 cancer patients from a palliative care unit; Chronic/acute pain: not stated Age 47.03 ± 16.46; Gender (female) 31 (51.7%); Primary cancer site: breast (16.7%), bone (18.3%), lungs (10%), hepatopancreatic (6.6%), esophageal (3.3%), nasopharyngeal (10%), prostate (5%), testicular (5%), brain (3.3%), cervical (1.7%), other (20%) | 5-min mindful breathing (n = 30) Control: 5-min normal listening (list of semi-structured questions) (n = 30) Professional: psychiatrist trained in mindfulness therapy | Pretreatment and posttreatment T1: beginning of session, T2: immediately after completion of the session, T3: 5–10 min after completion session | 10-point analog scale; 0 = no pain at all, 10 = severe pain | Student’s t-test (within group T1–T2, T1–T3) Mann–Whitney (between group T1–T2, T1–T3) | Intervention group: T1: 4.12 ± 2.62, T2: 3.65 ± 2.5, T3: 3.48 ± 2.49, T1–T2: p = 0.46, T1–T3: p = 0.32 Control group: T1: 4.17 ± 2.62, T2: 3.93 ± 2.37, T3: 3.93 ± 2.37, T1–T2: p = 0.72, T1–T3: p = 0.72 Between-group analysis were not done as reduction of pain within group was not statistically significant |
| Look et al.26 2020 Malaysia | Randomized controlled trial | 40 palliative care inpatients; Chronic/acute pain: not stated Intervention/control: Age: 66.75 ± 3.22/69.2 ± 2.54, Gender (female): 9 (45%)/11 (55%); Diagnosis: hepatobiliary and gastrointestinal malignancy 8 (40%)/8 (40%), lung malignancy 0/2 (10%), urological malignancy 1 (5%)/3 (15%), breast malignancy 1 (5%)/3 (15%), gynecological malignancy 3 (15%)/2 (10%), endocrine malignancy 1 (5%)/0, musculoskeletal malignancy 1 (5%)/0, nonmalignant 5 (25%)/1 (5%) | Single session 20-min mindful breathing: 4× 5-min guided breathing exercises with instructions to relax their body, focus their attention on their breathing and redirect attention back to their breathing when distracted (n = 20) Control group: 20-min conversation (n = 20) Professional: investigator | Pretreatment and posttreatment | ESAS (0–10); 0 = no symptoms, 10 = worst possible severity | Wilcoxon signed-rank test Mann–Whitney U test | Intervention group [median ((IQR))]: Pretest: 3.0 (4), Posttest 2.5 (6), p = 0.468 Control group: Pretest: 1.0 (5), Posttest: 2.0 (5), p = 0.152 Mean rank: Intervention: 23.2, Control: 17.8, p = 0.149 |
| Beng et al.25 2018 Malaysia | Randomized controlled study | 40 palliative care inpatients; Chronic/acute pain: not stated Intervention/control: Age: 56.9 ± 10.98/58.1 ± 14.53, Gender (female): 12/12 | 20-min mindful breathing Control group: 20-min supportive listening with semi-structured questions Professional: research assistants (MD) | T1: baseline, T2: during 5 min, T3: at 5 min, T4: during 20 min, T5: at 20 min | Numerical rating scale (0–10); 0 = no pain, 10 = worst possible pain | Independent samples t-test (between groups) Repeated measures analysis of variance (pairwise comparisons) | Intervention group: T1: 4.10 ± 2.67, T2: 2.45 ± 2.21, T3: 2.75 ± 2.29, T4: 1.85 ± 1.95, T5: 2.00 ± 2.10 Control group: T1: 3.35±3.39 T2: 3.00±2.99 T3: 2.95 ± 2.98 T4: 2.85 ± 2.96 T5: 2.95 ± 2.98 p-Values comparisons: T1(0.44), T2(0.51), T3(0.81), T4(0.22), T5(0.25) Mean difference (p): T2–T1: −1.65 (0.01), T3–T1: −1.35 (0.01), T4–T1: −2.25(0.00), T5–T1: −2.10 (0.00) Statistically significant reduction of pain score in the mindful breathing group but not in the control group |
| Anderson et al.33 2006 United States | Randomized controlled trial | 57 ambulatory outpatients with cancer; Chronic/acute pain: chronic cancer-related pain Age 52 (30–80); Gender (female) 45 (79%); Primary cancer site: breast (38), prostate (5), multiple myeloma (8), lung (6) | Cognitive-behavioral audiotapes interventions: Positive mood group: 20-min audiotape including positive mood statements and positive imagery suggestions Relaxation group: 20-min audiotape including standard progressive muscle-relaxation instructions Distraction group: 20-min audiotape including topics as history, foreign language, geography, or vocabulary Waiting-list group: offered a choice of audiotapes from the other groups at third assessment (4–5 weeks after baseline) Professional: self-applied by patients | Pretreatment and posttreatment Follow-up T1 (baseline), T2 (week 2–3), T3 (week 4–5), T4 (week 8–9) | 0–10 scale BPI (0–10 scale): change in BPI ‘worst pain’ ratings from T1 to T2 | Paired t-test ANOVA across four time points | Mean reduction in pain scores: Distraction group: 1.16 (95% CI: 0.47, 1.85; p = 0.004) Relaxation group: 0.9 (95% CI: 0.16, 1.65; p = 0.023) Positive mood group: −0.08 (95% CI: −1.53, 0.138; p = 0.91) Pairwise comparisons at each time point indicated no significant differences between groups |
| De Paolis et al.31 2018 Italy | Randomized controlled Non-pharmacological trial | 104 hospice patients; Chronic/acute pain: not stated Age 71.83 ± 11.57; Gender (female) 54 (48.07%); Primary cancer site: breast (7), gastrointestinal tract (22), genitourinary apparatus (18), reproductive organs (5), head and neck (6), lung (12), liver and pancreas (24), blood (1), other (8). | 20-min PMR-IGI sessions (n = 46): 4-min prolonged deep breathing and relaxation of the main muscle groups (PMR) Patients chooses script (e.g. walk along deserted beach, through woods), closing of the eyes, practitioner uses questions and prompts to participate in the scene (hear, smell, touch, taste), opening of the eyes, and contact with surroundings Control group: usual care (n = 45) Professional: practitioner experienced with guided imagery | Pretreatment and posttreatment | NRS (0–10); 0 = no symptom, 10 = worst possible symptom intensity PID (NRS pretreatment–NRS posttreatment) | Paired t-test | PMR-IGI: Pretest: 4.11 ± 2.05, Posttest: 2.28 ± 2.15, PID: 1.83 Control group: Pretest: 4.51 ± 2.39, Posttest: 3.96 ± 3.04, PID: 0.55 PID was significant (p < 0.0001) in both groups. The average value suggests a greater effect of the intervention group compared with usual care |
| Brugnoli et al.34 2018 Italy | Non-randomized clinical trial | 50 outpatients of the pain therapy clinic; Chronic/acute pain: chronic Intervention group/Control group: Age 61 ± 13/67 ± 14, Gender(female) 19 (76%)/17 (68%); Diagnosis (severe chronic): Rheumatic 11 (44%)/10 (40%), Neurologic 7 (28%)/9 (36%), Cancer 7 (28%)/6 (24%) | 1 and 2-years follow-up, both conventional pharmacological therapies. Hypnosis group: clinical and self-hypnosis (n = 25); Control group: usual care (n = 25) Techniques used: exercise ‘warm hands’, transferred symptoms techniques, positive visualization technique, desensitization of pain technique, self-hypnosis technique, self-hypnosis CD method Professional: primary investigator (MD) | Baseline, 1 year follow-up and 2 years follow-up | VAS (0–100 mm); 0 = no pain, 100 = worst imaginable pain Opioid use: yes/no | Students t-test ANOVA Chi-square test | Hypnosis group: Baseline: 81.9 ± 14.6, 1 year: 45.9 ± 13.8, 2 years: 38.9 ± 12.4 Control group: Baseline: 78.5 ± 14.8, 1 year: 62.1 ± 15.4, 2 years: 57.1 ± 15.9 Variance analysis indicated that the decrease in perceived pain was more significant (p = 0.0001) in the hypnosis group patients after 1- and 2-year follow-up Hypnosis therapy was associated with a decreased risk of 66% of needing to increase the opioids treatment for pain control (p = 0.03) |
| Lefèvre et al.27 2020 France | Mixed-method quasi-experimental | 20 palliative care patients on palliative care unit; Chronic/acute pain: not stated Age 57.9 ± 11.5; Gender (female): 14 (80%); Primary cancer site: gastrointestinal (25%), breast (15%), blood (15%), melanomas (15%), head and neck (10%), urological (10%), other (10%) | Art therapy session using techniques: painting, drawing, photography, modeling, and sculpture. Patients choose technique and topic and could be assisted by a family member if they wished. Focus was on orientating the patient toward a positive affective state. Professional: art therapist | Pretreatment (5-min before) and posttreatment (5-min after) | ESAS (0–10); 0 = no pain, 10 = worst imaginable pain | Wilcoxon’s test for paired sample | Pain improved from a median of 2 to a median of 1.3 (p < 0.001) Art therapy sessions significantly reduced pain (−42%, Cohen’s d = 0.59) |
| Collette et al.28 2020 Spain | Pre-post single-arm intervention study | 80 advanced cancer patients on tertiary hospital palliative care unit; Chronic/acute pain: not stated Age 60.2 ± 12.7; Gender (female): 41 (49%); Primary cancer site: colorectal 19 (22.9%), lung 14 (16.9%), breast 8 (9.6%), prostate 7 (8.4%), pancreas 5 (6%), hematologic 5 (6%), ovary 4 (4.8%), bone/soft tissues 4 (4.8%), other 17 (20.5%) | 60-min daily/alternate-days art therapy consisting of drawing, painting, collage, and modeling. Professional: art therapist | Pretreatment and posttreatment Before the sessions, T1 after first session, T3 after third session, T5 after fifth session | ESAS (VAS); 10 = most severe pain | Wilcoxon signed-rank test | T1 pretest: 3.05, T1 posttest: 2.75, T3 pretest: 2.93, T3 posttest: 2.34, T5 pretest: 2.27, T5 posttest: 1.67 p < 0.005 is all pre–post comparisons |
| Yamamoto et al.35 2011 Japan | Pilot experimental design | 18 hospitalized patients with incurable cancer; Chronic/acute pain: chronic Intervention group/Control group: Age 50–59 (2/3); 60–69 (5/3), ⩾70 (2/3); Gender (female) (3/3); Primary cancer site: gastric (0/3), colon (2/2), liver (1/2), pancreatic (2/0), breast (0/1), uterine (1/0), bronchogenic (2/0), chronic myelogenous leukaemia (1/1) | Wrapped warm footbath procedure (n = 9): lower legs and feet rubbed with olive oil (5 min), soak feet, modulation hot water 38°C and patient’s legs wrapped with plastic bag and cover legs with blanket (20 min), wash feet with foamy body shampoo using cotton gloves (5 min). Control group (n = 9): rest in recumbent position for 80 min. Professional: not stated | Pretreatment, three different treatment periods (different stages intervention), posttreatment | VAS (0–100 mm); 0 = painless, 100 = pain | Paired t-test | Footbath Pretest: 4.11 ± 2.58; Posttest: 1.78 ± 1.82; T(2.347), p = 0.047; average VAS decreased significantly Control group: Pretest: 2.44 ± 2.30; Posttest: 2.54 ± 2.54; T(−0.245), p = 0.813 |
| Sikorskii et al.36 2020 United States | Randomized controlled trial | 209 patients with advanced breast cancer; Chronic/acute pain: not stated Intervention group/Control group: Age 58.95 ± 11.32/55.54 ± 10.08; Metastatic (yes) 59 (58%)/66 (62%); Recurrent (yes) 31 (30%)/30 (28%) | 30-min home-based reflexology session (n = 102): applying of firm walking motion pressure to specific areas on the feet referred to as reflexes (15 min/foot). At least one per week (for 4 weeks) Control group (n = 107): attention control Professional: caregivers | Weekly symptom assessment | MD Anderson Symptom Inventory (0–10); 0 = not present, 10 = as bad as you can imagine Cutoff points: 1 = mild, 2–4 = moderate, 5–10 = severe | Responders: Moved from (onset to last symptom assessment) - severe to moderate/mild - moderate to mild/none - remained mild Nonresponders: - mild to moderate/severe - moderate to severe - remained severe Odds ratios | Response/nonresponse (%) Reflexology: Severe (n = 44) 72/27, Moderate (n = 40) 38/62, Mild (n = 18) 100/0 Control: Severe (n = 44) 55/45, Moderate (n = 48) 29/71, Mild (n = 15) 100/0 Reflexology was more successful than attention control in producing response for pain. Odds ratio = 1.84; 95% CI: 1.05, 3.23; p = 0.03. |
| Niki et al.37 2019 Japan | Prospective multicenter, single-arm study | 20 patients with terminal cancer from two palliative care wards; Chronic/acute pain: not stated Age 72.3 ± 11.9; Gender (female) 6 (30%); Primary cancer site: pancreas (3), uterus (2), lung (2), head and neck (2), prostate (2), kidney (2), biliary duct (2), other (5) | 30-min VR travel session with VR headset HTC VIVE and free VR software Google Earth VR® Professional: self-applied by patients | Pretreatment and posttreatment | ESAS | Paired t-test For detecting moderate/severe symptoms the cutoff value is ⩾3 for pain | Before VR travel: 2.35 ± 2.25 After VR travel: 1.15 ± 2.03 (p = 0.005) Moderate/severe pain: Before VR travel (n = 10) 30%; After VR travel (n=3) 15% Significant improvement on pain for n = 15 (75%) that went to memorable places (p = 0.018). No significant improvements for n = 5 who went to places desired to visit, but never visited (p = 0.317). |
| Moscato et al.38 2021 Italy | Pre-post single-arm study | 14 advanced cancer patients assisted within home-palliative care program; Chronic/acute pain: not stated Age 47.2 ± 14.2; Gender (female) 11 (78.6%); Primary cancer site: gastrointestinal (4), genital tract (2), hematological (2), breast (2), urinary (2), bone and soft tissues (1), endocrine (1) | At least one session of mirage sole VR with interactive and noninteractive contents. Noninteractive: immersive 360° videos with different natural and relaxing scenarios, such as a seascape, a park e.g. Interactive: basic skill game ‘Yuma’s world’ Average of 55 min per participant. Minimum of one session of 3 min Professional: self-applied by patients | Pretreatment and posttreatment | ESAS | Wilcoxon signed-rank test | T0: 1.06 ± 0.25, T1: 0.66 ± 0.1 Difference pre- and posttest: −37.73% (p ⩽ 0.01) |
| Krishnaswamy et al.39 2016 India | Comparative pilot study | 14 cancer patients at a palliative care ward; Chronic/acute pain: not stated Intervention group/control group: Gender (female): 5 (71%)/3 (43%) | 20-min music (instrumental music – Veena and Flute: combination of traditional Indian raga Anandabhairavi and modern contemporary tune) administered by headphones and MP3 player Control group: kept occupied with 20 min of talking to them Professional: self-applied by patients | Pretreatment and posttreatment | NRS (0–10); 0 = no pain, 10 = worst pain imaginable | Students t-test Two-sample t-test | Music Pretest: 5.43 ± 1.27, Posttest: 4.00 ± 1.29, Decrease 1.43 ± 0.78; Statistically significant (p = 0.003) Control Pretest: 5.86 ± 1.21; Posttest 5,71 ± 1.38; Decrease 0.14 ± 0.38; Not statistically significant (p = 0.356) Difference between groups: −1.71 ± 0.71. Statistically significant (p = 0.034) |
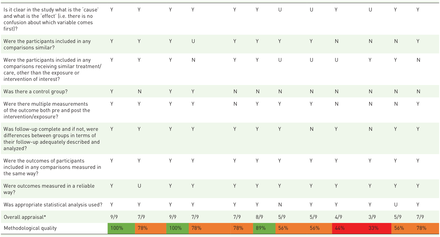
| Questions checklist RCT | Yamamoto et al.35 | Sikorskii et al.36 | Soden et al.29 | Anderson et al.33 | Kutner et al.18 | De Paolis et al.31 | Wilkie et al.19 | Guan et al.24 | Look et al.26 | Beng et al.25 |
|---|---|---|---|---|---|---|---|---|---|---|
 | ||||||||||
| Brugnoli et al.34 | Louis and Kowalsk30 | Lee et al.32 | Krishnaswamy and Nair39 | Jane et al.22 | Niki et al.37 | Mitchinson et al.21 | Lefèvre et al.27 | Pedersen and Björkhem-Bergman23 | Collette et al.28 | Havyer et al.20 | Moscato et al.38 | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
 | ||||||||||||
Mind–body interventions
Mindful breathing
Art therapy
Progressive muscle-relaxation and interactive guided imagery
MBSR program
Cognitive-behavioral audiotapes
Hypnosis
Virtual reality
Music therapy
Biologically based treatments
Aromatherapy
Manipulative and body-based practices
Massage
Wrapped warm footbath
Reflexology
Best-evidence synthesis
| Intervention | Methodological quality per study | Level of evidence* |
|---|---|---|
 | ||
Discussion
Main findings
Implications for practice
Comparisons with literature
Strengths and limitations
Conclusion
Acknowledgments
ORCID iDs
Footnotes
Appendix
| PubMed | Search |
|---|---|
| Domain (#1) | ‘palliative care’[MeSH Terms] OR ‘Hospice and Palliative Care Nursing’[MeSH Terms] OR ‘Palliative Medicine’[MeSH Terms] OR ‘Terminal Care’[MeSH Terms] OR ‘end of life’[Tiab] OR ‘palliation’[Tiab] OR ‘palliative*’[Tiab] OR ‘hospice*’[Tiab] OR ‘terminal care’[Tiab] OR ‘advanced care’ OR ‘terminally ill’[MeSH Terms] OR ‘terminally ill’[Tiab] |
| Determinant (#2) | (‘oils, volatile’[MeSH Terms] OR (‘oils’[Tiab] AND ‘volatile’[Tiab]) OR ‘volatile oils’[Tiab] OR (‘essential’[Tiab] AND ‘oils’[Tiab]) OR ‘essential oils’[Tiab]) OR (‘acupressure’[MeSH Terms] OR ‘acupressure’[Tiab]) OR biofield[Tiab] OR (‘therapeutic touch’[MeSH Terms] OR (‘therapeutic’[Tiab] AND ‘touch’[Tiab]) OR ‘therapeutic touch’[Tiab] OR ‘reiki’[Tiab]) OR (‘cognitive behaviour therapy’[Tiab] OR ‘cognitive behavioral therapy’[MeSH Terms] OR ‘cognitive behavioral therapy’[Tiab] OR ‘cognitive behavior therapy’[Tiab]) OR (‘biofeedback, psychology’[MeSH Terms] OR ‘biofeedback’[Tiab]) OR (‘phototherapy’[MeSH Terms] OR ‘phototherapy’[Tiab] OR (‘light’[Tiab] AND ‘therapy’[Tiab]) OR ‘light therapy’[Tiab]) OR (‘hypnosis’[MeSH Terms] OR ‘hypnosis’[Tiab]) OR (‘musculoskeletal manipulations’[MeSH Terms] OR (‘musculoskeletal’[Tiab] AND ‘manipulations’[Tiab]) OR ‘musculoskeletal manipulations’[Tiab] OR ‘reflexology’[Tiab]) OR ((‘relaxation’[MeSH Terms] OR ‘relaxation’[Tiab]) AND (‘exercise’[MeSH Terms] OR ‘exercise’[Tiab])) OR ((‘abdomen’[MeSH Terms] OR ‘abdomen’[Tiab] OR ‘abdominal’[Tiab]) AND (‘respiration’[MeSH Terms] OR ‘respiration’[Tiab] OR ‘breathing’[Tiab])) OR (‘autogenic training’[MeSH Terms] OR (‘autogenic’[Tiab] AND ‘training’[Tiab]) OR ‘autogenic training’[Tiab] OR (‘progressive’[Tiab] AND ‘muscle’[Tiab] AND ‘relaxation’[Tiab]) OR ‘progressive muscle relaxation’[Tiab]) OR ((‘imagery, psychotherapy’[MeSH Terms] OR (‘imagery’[Tiab] AND ‘psychotherapy’[Tiab]) OR ‘imagery’[Tiab]) AND (‘education’[Subheading] OR ‘education’[Tiab] OR ‘training’[Tiab] OR ‘education’[MeSH Terms] OR ‘training’[Tiab])) OR (‘meditation’[MeSH Terms] OR ‘meditation’[Tiab]) OR (‘yoga’[MeSH Terms] OR ‘yoga’[Tiab]) OR (‘music’[MeSH Terms] OR ‘music’[Tiab]) OR (‘massage’[MeSH Terms] OR ‘massage’[Tiab]) OR (‘aromatherapy’[MeSH Terms] OR ‘aromatherapy’[Tiab]) OR (‘odorants’[MeSH Terms] OR ‘odorants’[Tiab] OR ‘aroma’[Tiab]) OR (‘mindfulness’[MeSH Terms] OR ‘mindfulness’[Tiab]) OR (‘diet’[MeSH Terms] OR ‘diet’[Tiab] OR ‘diets’[Tiab]) OR (‘art’[MeSH Terms] OR ‘art’[Tiab]) OR psychoeducation[Tiab] OR herbs[Tiab] OR (‘dietary supplements’[MeSH Terms] OR (‘dietary’[Tiab] AND ‘supplements’[Tiab]) OR ‘dietary supplements’[Tiab] OR (‘nutritional’[Tiab] AND ‘supplements’[Tiab]) OR ‘nutritional supplements’[Tiab]) OR (‘homeopathy’[MeSH Terms] OR ‘homeopathy’[Tiab] OR ‘homoeopathy’[Tiab] OR ‘homeopathic’[Tiab]) OR ‘shiatsu’[Tiab] OR (‘virtual reality’[MeSH Terms] OR ‘virtual reality’[Tiab]) OR ‘color therapy’[Tiab] OR (‘color*’[Tiab] AND ‘therapy’[Tiab]) OR ‘acoustic stimulation’ [Tiab] OR ‘acoustic stimulation’ [MeSH Terms] OR ‘auditory stimulation’ [Tiab] OR ((‘acoustic’ [Tiab] OR ‘auditory’ [Tiab]) AND (‘therapy’[Tiab] OR ‘stimulation’[Tiab])) OR complementary[Tiab] OR complementary[Tiab] OR ((‘complementary’ [Tiab] AND ‘alternative’ [Tiab] AND ‘medicine’[Tiab]) OR ‘complementary alternative medicine’[Tiab]) OR (‘complementary therapies’[MeSH Terms] OR ‘complementary therapies’[Tiab]) |
| Outcome (#3) | ((‘pain’[MeSH terms] OR ‘pain*’[Tiab] OR ‘discomfort*’[Tiab] OR ‘ache*’[Tiab] OR ‘aching’[Tiab] OR ‘sore*’[Tiab] OR ‘suffer*’[Tiab] OR ‘agony’[Tiab] OR ‘hurt*’[Tiab] OR ‘strain’[Tiab] OR ‘torment’[Tiab] OR ‘twinge’[Tiab] OR ‘symptom’[Tiab] OR ‘symptom burden’[Tiab] OR (‘symptom’[Tiab] AND ‘burden’[Tiab])) AND (assess*[Tiab] OR relief[Tiab] OR reliev*[Tiab] OR reduc*[Tiab])) |
| Embase (not MEDLINE) | Search |
| Domain (#1) | ‘palliative nursing’/exp OR ‘palliative therapy’/exp OR ‘terminal care’/exp OR ‘end of life care’:ti,ab OR ‘palliation’:ti,ab OR ‘palliative*’:ti,ab OR ‘hospice*’:ti,ab OR ‘terminal care’:ti,ab OR ‘terminally ill patient’/exp OR ‘terminally ill’:ti,ab OR ‘advance care’:ti,ab |
| Determinant (#2) | ‘essential oil’/exp OR ‘essential oil’:ab,ti OR (‘oils’:ab,ti AND ‘volatile’:ab,ti) OR ‘acupressure’/exp OR ‘acupressure’:ab,ti OR ‘biofield therapy’/exp OR ‘biofield therapy’:ab,ti OR ‘therapeutic touch’/exp OR ‘therapeutic touch’:ab,ti OR ‘reiki’/exp OR ‘reiki’:ab,ti OR ‘cognitive behavioral therapy’/exp OR ‘cognitive behavioral therapy’:ab,ti OR ‘biofeedback’/exp OR ‘biofeedback’:ab,ti OR ‘phototherapy’/exp OR ‘phototherapy’:ab,ti OR (‘light’:ab,ti AND ‘therapy’:ab,ti) OR ‘hypnosis’/exp OR ‘hypnosis’:ab,ti OR ‘musculoskeletal manipulation’/exp OR ‘musculoskeletal manipulation’:ab,ti OR (‘musculoskeletal’:ab,ti AND ‘manipulation’:ab,ti) OR ‘reflexology’:ab,ti OR ‘relaxation training’/exp OR ‘relaxation training’:ab,ti OR ‘abdominal breathing’/exp OR ‘abdominal breathing’:ab,ti OR ‘autogenic training’/exp OR ‘autogenic training’:ab,ti OR ‘progressive muscle relaxation’/exp OR ‘progressive muscle relaxation’ OR ‘sleep hygiene’/exp OR ‘sleep hygiene’:ab,ti OR ‘imagery training’:ab,ti OR ((‘imagery’/exp OR imagery:ab,ti) AND (‘training’/exp OR training:ab,ti)) OR ‘meditation’/exp OR ‘meditation’:ab,ti OR ‘yoga’/exp OR ‘yoga’:ab,ti OR ‘music therapy’/exp OR ‘music therapy’:ab,ti OR ‘massage’/exp OR ‘massage’:ab,ti OR ‘aromatherapy’/exp OR ‘aromatherapy’:ab,ti OR ‘fragrance’/exp OR ‘fragrance’:ab,ti OR ‘aroma’/exp OR ‘aroma’:ab,ti OR ‘mindfulness’/exp OR ‘mindfulness’:ab,ti OR ‘diet’/exp OR ‘diet’:ab,ti OR ‘art’/exp OR ‘art’:ab,ti OR ‘psychoeducation’/exp OR ‘psychoeducation’:ab,ti OR ‘herb’/exp OR ‘herb:ab,ti OR ‘dietary supplement’/exp OR ‘dietary supplement’:ab,ti OR ‘nutritional supplements’:ab,ti OR (‘nutritional‘:ab,ti AND ‘supplements‘:ab,ti) OR ‘homeopathy‘/exp OR ‘homeopathy‘:ab,ti OR ‘shiatsu’/exp OR ‘shiatsu’:ab,ti OR ‘virtual reality’/exp OR ‘virtual reality’:ab,ti OR ‘color therapy’/exp OR ‘color therapy’:ab,ti OR (‘color*’:ab,ti AND ‘therapy’:ab,ti) OR ‘auditory stimulation’/exp OR ‘auditory stimulation’:ab,ti OR ((‘auditory’:ab,ti OR ‘acoustic’:ab,ti) AND (‘stimulation’:ab,ti OR ‘therapy’:ab,ti)) complementary:ab,ti OR ‘complementary alternative medicine’:ab,ti OR (complementary:ab,ti AND alternative:ab,ti AND (‘medicine‘/exp OR medicine:ab,ti)) OR ‘alternative medicine’/exp OR ‘alternative medicine’:ab,ti |
| Outcome (#3) | ((‘pain’/exp OR ‘pain*’:ab,ti OR ‘discomfort’:ab,ti OR ‘suffer*’:ti,ab OR ‘ache*’:ti,ab OR ‘aching’:ab,ti OR ‘sore*’:ab,ti OR ‘agony’:ti,ab OR ‘hurt*’:ti,ab OR ‘strain*’:ti,ab OR ‘torment*’:ti,ab OR ‘twinge’:ti,ab OR ‘symptom*’:ab,ti OR ‘symptom burden’:ab,ti) AND (‘assess*’:ab,ti OR ‘relief’:ab,ti OR ‘reliev*’:ab,ti OR ‘reduc*’:ab,ti)) |
| CINAHL | Search |
| Domain (#1) | MH ((MH ‘Terminal care’) OR (MH ‘Hospice care’) OR (MH ‘Palliative care’) OR (MH ‘Hospice and Palliative Nursing’)) OR TI (‘end of life care’ OR ‘palliation’ OR ‘palliative*’ OR ‘hospice*’ OR ‘terminal care’ OR ‘terminally ill’ OR ‘advance care’) OR AB (‘end of life care’ OR ‘palliation’ OR ‘palliative*’ OR ‘hospice*’ OR ‘terminal care’ OR ‘terminally ill’ OR ‘advance care’) |
| Determinant (#2) | MH (MH ‘essential oils’) OR (MH ‘acupressure’) OR (MH ‘therapeutic touch’) OR (MH ‘reiki’) OR (MH ‘phototherapy’) OR (MH ‘hypnosis’) OR (MH ‘reflexology’) OR (MH ‘progressive muscle relaxation’) OR (MH ‘guided imagery’) OR (MH ‘meditation’) OR (MH ‘yoga’) OR (MH ‘music therapy’) OR (MH ‘music’) OR (MH ‘massage’) OR (MH ‘aromatherapy’) OR (MH ‘odors’) OR (MH ‘mindfulness’) OR (MH ‘diet’) OR (MH ‘art’) OR (MH ‘psychoeducation’) OR (MH ‘dietary supplements’) OR (MH ‘homeopathy’) OR (MH ‘shiatsu’) OR (MH ‘virtual reality’) OR (MH ‘acoustic stimulation’) OR (MH ‘alternative therapies’) OR (MH (MH ‘relaxation’) OR TI (‘relaxation’) OR AB (‘relaxation’)) AND (TI (‘exercise*’) OR AB (‘exercise*’)) OR (MH (MH ‘abdomen’) OR TI (‘abdomen’ OR ‘abdominal’) OR AB (‘abdomen’ OR ‘abdominal’)) AND (MH (MH ‘respiration’) OR TI (‘respiration’ OR ‘breathing’) OR AB (‘respiration’ OR ‘breathing’)) OR (MH (MH ‘autogenic training’) OR TI (‘autogenic’ AND ‘training’) OR ‘autogenic training’ OR AB (‘autogenic’ AND ‘training’) OR ‘autogenic training’) OR ((MH (MH ‘guided imagery’) OR TI (‘psychotherapy imagery’ OR (‘psychotherapy’ AND ‘imagery’) OR ‘imagery’) OR AB (‘psychotherapy imagery’ OR (‘psychotherapy’ AND ‘imagery’) OR ‘imagery’)) AND (MH (MH ‘education’) OR TI (‘education’ OR ‘training’) OR AB (‘education’ OR ‘training’))) OR TI (‘volatile oils’ OR (‘oils’ AND ‘volatile’) OR ‘essential oils’ OR (‘essential’ AND ‘oils’) OR ‘acupressure’ OR ‘biofield’ OR ‘therapeutic touch’ OR (‘therapeutic’ AND ‘touch’) OR ‘reiki’ OR ‘cognitive behaviour therapy’ OR ‘cognitive behavioural therapy’ OR ‘biofeedback’ OR ‘phototherapy’ OR (‘light’ AND ‘therapy’) OR ‘light therapy’ OR ‘hypnosis’ OR ‘musculoskeletal manipulations’ OR (‘musculoskeletal’ AND ‘manipulations’) OR ‘reflexology’ OR (‘progressive’ AND ‘muscle’ AND ‘relaxation’) OR ‘progressive muscle relaxation’ OR ‘meditation’ OR ‘yoga’ OR ‘music therapy’ OR ‘music’ OR ‘massage*’ OR ‘aromatherapy’ OR ‘odors’ OR ‘odorants’ OR ‘aroma’ OR ‘mindfulness’ OR ‘diet’ OR ‘diets’ OR ‘art*’ OR ‘psychoeducation’ OR ‘herbs’ OR ‘dietary supplement*’ OR (‘dietary’ AND ‘supplement*’) OR (‘nutritional’ AND ‘supplement*’) OR ‘nutritional supplements’ OR ‘homeopathy’ OR ‘homoeopathy’ OR ‘homeopathic’ OR ‘shiatsu’ OR ‘virtual reality’ OR (‘virtual’ AND ‘reality’) OR ‘color therapy’ OR (‘color’ AND ‘therapy’) OR ‘acoustic stimulation’ OR (‘acoustic’ AND (‘stimulation’ OR ‘therapy’)) OR ‘auditory stimulation’ OR (‘auditory’ AND (‘stimulation’ OR ‘therapy’)) OR ‘alternative therapy’ OR ‘alternative therapies’ OR ‘complementary’ OR (‘complementary’ AND ‘alternative’ AND ‘medicine’) OR ‘complementary alternative medicine’ OR ‘complementary therapy’ OR ‘complementary therapies’) OR AB (‘volatile oils’ OR (‘oils’ AND ‘volatile’) OR ‘essential oils’ OR (‘essential’ AND ‘oils’) OR ‘acupressure’ OR ‘biofield’ OR ‘therapeutic touch’ OR (‘therapeutic’ AND ‘touch’) OR ‘reiki’ OR ‘cognitive behaviour therapy’ OR ‘cognitive behavioural therapy’ OR ‘biofeedback’ OR ‘phototherapy’ OR (‘light’ AND ‘therapy’) OR ‘light therapy’ OR ‘hypnosis’ OR ‘musculoskeletal manipulations’ OR (‘musculoskeletal’ AND ‘manipulations’) OR ‘reflexology’ OR (‘progressive’ AND ‘muscle’ AND ‘relaxation’) OR ‘progressive muscle relaxation’ OR ‘meditation’ OR ‘yoga’ OR ‘music therapy’ OR ‘music’ OR ‘massage*’ OR ‘aromatherapy’ OR ‘odors’ OR ‘odorants’ OR ‘aroma’ OR ‘mindfulness’ OR ‘diet’ OR ‘diets’ OR ‘art*’ OR ‘psychoeducation’ OR ‘herbs’ OR ‘dietary supplement*’ OR (‘dietary’ AND ‘supplement*’) OR (‘nutritional’ AND ‘supplement*’) OR ‘nutritional supplements’ OR ‘homeopathy’ OR ‘homoeopathy’ OR ‘homeopathic’ OR ‘shiatsu’ OR ‘virtual reality’ OR (‘virtual’ AND ‘reality’) OR ‘color therapy’ OR (‘color’ AND ‘therapy’) OR ‘acoustic stimulation’ OR (‘acoustic’ AND (‘stimulation’ OR ‘therapy’)) OR ‘auditory stimulation’ OR (‘auditory’ AND (‘stimulation’ OR ‘therapy’)) OR ‘alternative therapy’ OR ‘alternative therapies’ OR ‘complementary’ OR (‘complementary’ AND ‘alternative’ AND ‘medicine’) OR ‘complementary alternative medicine’ OR ‘complementary therapy’ OR ‘complementary therapies’) |
| Outcome (#3) | ((MH (MH ‘pain’) OR TI (‘pain*’ OR ‘discomfort’ OR ‘suffer*’ OR ‘ache*’ OR ‘aching’ OR ‘sore’ OR ‘agony’ OR ‘hurt*’ OR ‘strain*’ OR ‘torment*’ OR ‘twinge’ OR ‘symptom’ OR ‘symptom burden’) OR AB (‘pain*’ OR ‘discomfort’ OR ‘suffer*’ OR ‘ache*’ OR ‘aching’ OR ‘sore’ OR ‘agony’ OR ‘hurt*’ OR ‘strain*’ OR ‘torment*’ OR ‘twinge’ OR ‘symptom’ OR ‘symptom burden’) AND (TI (‘asses*’ OR ‘relief’ OR ‘reliev*’ OR ‘reduc*’) OR AB (‘asses*’ OR ‘relief’ OR ‘reliev*’ OR ‘reduc*’))) |
| Psycinfo | Search |
| Domain (#1) | exp Palliative Care/ OR exp Alternative Medicine/ OR exp Hospice/ OR exp Terminally ill patients/ OR palliative care.ti,ab. OR terminal care.ti,ab. OR end of life.ti,ab. OR palliation.ti,ab. OR palliative*.ti,ab. OR hospice*.ti,ab. OR advance care.ti,ab. OR terminally ill.ti,ab. |
| Determinant (#2) | exp Aromatherapy/ OR exp Cognitive behavior therapy/ OR exp Biofeedback/ OR exp Phototherapy/ OR exp Hypnosis/ OR exp Autogenic Training/ OR exp Progressive Relaxation Therapy/ OR exp Guided Imagery/ OR exp Imagery/ OR exp Meditation/ OR exp Yoga/ OR exp Music Therapy/ OR exp Massage/ OR exp Aromatherapy/ OR exp Mindfulness/ OR exp Diets/ OR exp Art Therapy/ OR exp Psychoeducation/ OR exp Medicinal Herbs and Plants/ OR exp Dietary Supplements/ OR exp Virtual Reality/ OR exp Auditory Stimulation/ OR volatile oils.ti,ab. OR (volatile AND oils).ti,ab. OR essential oils.ti,ab. OR (essential AND oils).ti,ab. OR acupressure.ti,ab. OR biofield.ti,ab. OR therapeutic touch.ti,ab. OR (therapeutic AND touch).ti,ab. OR reiki.ti,ab. OR cognitive behavior therapy.ti,ab. OR (cognitive AND behavior AND therapy).ti,ab. OR (cognitive AND behavioral AND therapy).ti,ab.OR cognitive behavioral therapy.ti,ab. OR (cognitive AND behaviour AND therapy).ti,ab. OR cognitive behaviour therapy.ti,ab. OR biofeedback.ti,ab. OR psychology biofeedback.ti,ab. OR (psychology AND biofeedback).ti,ab. OR phototherapy.ti,ab. OR light therapy.ti,ab. OR (light AND therapy).ti,ab. OR hypnosis.ti,ab. OR musculoskeletal manipulations.ti,ab. OR (musculoskeletal AND manipulations).ti,ab. OR reflexology.ti,ab. OR ((exp Relaxation/ OR relaxation.ti,ab.) AND (exp Exercise/ OR exercise*.ti,ab.)) OR ((exp Abdomen/ OR abdomen.ti,ab. OR abdominal.ti,ab. ) AND (exp Respiration/ OR respiration.ti,ab. OR breathing.ti,ab.)) OR autogenic training.ti,ab. OR (autogenic AND training).ti,ab. OR progressive muscle therapy.ti,ab. OR progressive muscle relaxation.ti,ab. OR (progressive AND muscle AND relaxation).ti,ab. OR (progressive AND relaxation AND therapy).ti,ab. OR ((guided imagery.ti,ab. OR psychotherapy imagery.ti,ab. OR (psychotherapy AND imagery).ti,ab. OR imagery.ti,ab.) AND (education.ti,ab. OR training.ti,ab.)) OR meditation.ti,ab. OR yoga.ti,ab. OR music therapy.ti,ab. OR (music AND therapy).ti,ab. OR massage*.ti,ab. OR aromatherapy.ti,ab. OR odorants.ti,ab. OR aroma.ti,ab. OR mindfulness.ti,ab. OR diet*.ti,ab. OR art*.ti,ab. OR art therapy.ti,ab. OR (art AND therapy).ti,ab. OR psychoeducation.ti,ab. OR herbs.ti,ab. OR dietary supplement*.ti,ab. OR (dietary AND supplement*).ti,ab. OR nutritional supplement*.ti,ab. OR (nutritional AND supplement*).ti,ab. OR homeopathy.ti,ab. OR homoeopathy.ti,ab. OR homeopathic.ti,ab. OR shiatsu.ti,ab. OR virtual reality.ti,ab. OR (virtual AND reality).ti,ab. OR acoustic stimulation.ti,ab. OR acoustic therapy.ti,ab. OR (acoustic AND (stimulation OR therapy)).ti,ab. OR (auditory AND (stimulation OR therapy)).ti,ab. OR complementary therapy.ti,ab. OR complementary.ti,ab. OR (complementary AND alternative AND medicine).ti,ab. OR complementary alternative medicine.ti,ab. OR complementary therapies.ti,ab |
| Outcome (#3) | (exp Pain/ OR pain.ti,ab. OR discomfort*.ti,ab. OR ache*.ti,ab. OR aching.ti,ab. OR sore*.ti,ab. OR suffer*.ti,ab. OR agony.ti,ab. OR hurts.ti,ab. OR strain.ti,ab. OR torment.ti,ab. OR twinge.ti,ab. OR symptom.ti,ab. OR (symptom AND burden).ti,ab. OR symptom burden.ti,ab.) AND (assess* OR relief OR reliev* OR reduc*).ti,ab. |
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
Cite
Cite
Cite
Download to reference manager
If you have citation software installed, you can download citation data to the citation manager of your choice
Information, rights and permissions
Information
Published In
Keywords
Authors
Metrics and citations
Metrics
Journals metrics
This article was published in Palliative Care and Social Practice.
View All Journal MetricsPublication usage*
Total views and downloads: 22628
*Publication usage tracking started in December 2016
Publications citing this one
Receive email alerts when this publication is cited
Web of Science: 18 view articles Opens in new tab
Crossref: 15
- Mindfulness-based interventions for pain, anxiety, depression, and quality of life in patients receiving palliative care: a meta-analysis
- Refractory bone pain in metastatic sarcoma: a multispecialty opioid-sparing approach to palliative care
- Prevention and Management of Wound Procedural Pain Management in Adult Patients with Open Wounds: Integration of the Latest Clinical Evidence
- Health-Related Quality of Life and Patient Experience in Oncology Palliative Care Within the Saudi Model of Care Framework: Evidence from the Qassim Health Cluster, Saudi Arabia
- Effect of vibration on pain during subcutaneous heparin injection: A randomized, single-blind, placebo-controlled trial
- Current status of knowledge, attitudes, and practices among ICU physicians and nurses regarding palliative care in China
- El uso de la tecnología para mejorar el cuidado de la salud mental en pacientes oncológicos: una revisión de alcance
- Pinwheel blowing and stress ball squeezing reduce children’s pain and anxiety during intravenous catheterization in a randomized controlled trial
- Nonpharmacological Methods and Pain Measurement Tools Used by Nurses Working in Surgical Clinics for Postoperative Pain Management
- Intersecting AI and Medicine for Improved Care and Administrative Efficiency
- View More
Figures and tables
Figures & Media
Tables
View Options
View options
PDF/EPUB
View PDF/EPUBAccess options
If you have access to journal content via a personal subscription, university, library, employer or society, select from the options below:
loading institutional access options
Alternatively, view purchase options below:
Access journal content via a DeepDyve subscription or find out more about this option.






